|
1
|
Vasilevska J, Cheng PF, Lehmann J, Ramelyte E, Gómez JM, Dimitriou F, Sella F, Ferretti D, Salas-Bastos A, Jordaan WS, Levesque MP, Dummer R, Sommer L. Monitoring melanoma patients on treatment reveals a distinct macrophage population driving targeted therapy resistance. Cell Rep Med 2024; 5:101611. [PMID: 38942020 PMCID: PMC11293307 DOI: 10.1016/j.xcrm.2024.101611] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 08/30/2023] [Revised: 04/09/2024] [Accepted: 05/20/2024] [Indexed: 06/30/2024]
Abstract
Resistance to targeted therapy remains a major clinical challenge in melanoma. To uncover resistance mechanisms, we perform single-cell RNA sequencing on fine-needle aspirates from resistant and responding tumors of patients undergoing BRAFi/MEKi treatment. Among the genes most prominently expressed in resistant tumors is POSTN, predicted to signal to a macrophage population associated with targeted therapy resistance (TTR). Accordingly, tumors from patients with fast disease progression after therapy exhibit high POSTN expression levels and high numbers of TTR macrophages. POSTN polarizes human macrophages toward a TTR phenotype and promotes resistance to targeted therapy in a melanoma mouse model, which is associated with a phenotype change in intratumoral macrophages. Finally, polarized TTR macrophages directly protect human melanoma cells from MEKi-induced killing via CD44 receptor expression on melanoma cells. Thus, interfering with the protective activity of TTR macrophages may offer a strategy to overcome resistance to targeted therapy in melanoma.
Collapse
Affiliation(s)
- Jelena Vasilevska
- Institute of Anatomy, University of Zurich, 8057 Zurich, Switzerland
| | - Phil Fang Cheng
- Department of Dermatology, University of Zurich Hospital and Faculty of Medicine, University of Zurich, Zurich, Switzerland
| | - Julia Lehmann
- Institute of Anatomy, University of Zurich, 8057 Zurich, Switzerland
| | - Egle Ramelyte
- Department of Dermatology, University of Zurich Hospital and Faculty of Medicine, University of Zurich, Zurich, Switzerland
| | - Julia Martínez Gómez
- Department of Dermatology, University of Zurich Hospital and Faculty of Medicine, University of Zurich, Zurich, Switzerland
| | - Florentia Dimitriou
- Department of Dermatology, University of Zurich Hospital and Faculty of Medicine, University of Zurich, Zurich, Switzerland
| | - Federica Sella
- Department of Dermatology, University of Zurich Hospital and Faculty of Medicine, University of Zurich, Zurich, Switzerland
| | - Daria Ferretti
- Institute of Anatomy, University of Zurich, 8057 Zurich, Switzerland
| | | | | | - Mitchell Paul Levesque
- Department of Dermatology, University of Zurich Hospital and Faculty of Medicine, University of Zurich, Zurich, Switzerland
| | - Reinhard Dummer
- Department of Dermatology, University of Zurich Hospital and Faculty of Medicine, University of Zurich, Zurich, Switzerland
| | - Lukas Sommer
- Institute of Anatomy, University of Zurich, 8057 Zurich, Switzerland.
| |
Collapse
|
|
2
|
Chen A, Wang K, Qi L, Hu W, Zhou B. Development of a novel prognostic signature for colorectal cancer based on angiogenesis-related genes. Heliyon 2024; 10:e33662. [PMID: 39040272 PMCID: PMC11261139 DOI: 10.1016/j.heliyon.2024.e33662] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/17/2024] [Revised: 06/20/2024] [Accepted: 06/25/2024] [Indexed: 07/24/2024] Open
Abstract
Background Colorectal cancer (CRC) is the third most common malignant tumor worldwide. Angiogenesis is closely related to tumor metastasis, which is the main cause of cancer death. Although several angiogenesis signatures have been proposed in some cancer types, no angiogenic signature has been developed to predict the prognosis and efficacy of antiangiogenic bevacizumab in CRC patients. Methods We developed a novel CRC angiogenic signature by refining seven publicly available angiogenic gene sets using least absolute shrinkage and selection operator (LASSO). Immune and stromal cells within the tumor microenvironment were compared between the high- and low-risk groups in more than 1000 CRC samples classified by calculating the risk score based on the customized angiogenic signature. The correlation of this new gene set with the efficacy of bevacizumab was also compared. Results A new prognostic-associated angiogenesis signature gene set was constructed that can divide CRC patients into two high- and low-risk groups. The high-risk angiogenic group was significantly associated with extracellular matrix organization, epithelial-mesenchymal transition (EMT), and myogenesis. In addition, the high-risk group had higher infiltration of stromal and immune cells and was more resistant to bevacizumab than the low-risk group. Conclusion Briefly, we constructed a novel angiogenic signature that can predict the prognosis of CRC patients and the efficacy of bevacizumab in treating CRC. Our results provide new insights into the relationships among angiogenesis, metastasis, and medication for CRC.
Collapse
Affiliation(s)
- Aiqin Chen
- Department of Nursing, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, 310009, China
| | - Kailai Wang
- Cancer Institute, Key Laboratory of Cancer Prevention and Intervention, Ministry of Education, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, China
- Department of Medical Oncology, Key Laboratory of Cancer Prevention and Intervention, Ministry of Education, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, 310009, China
- Cancer Center, Zhejiang University, Hangzhou, Zhejiang, 310058, China
| | - Lina Qi
- Cancer Institute, Key Laboratory of Cancer Prevention and Intervention, Ministry of Education, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, China
- Department of Medical Oncology, Key Laboratory of Cancer Prevention and Intervention, Ministry of Education, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, 310009, China
- Cancer Center, Zhejiang University, Hangzhou, Zhejiang, 310058, China
| | - Wangxiong Hu
- Cancer Institute, Key Laboratory of Cancer Prevention and Intervention, Ministry of Education, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, China
- Cancer Center, Zhejiang University, Hangzhou, Zhejiang, 310058, China
| | - Biting Zhou
- Cancer Institute, Key Laboratory of Cancer Prevention and Intervention, Ministry of Education, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, China
- Department of Medical Oncology, Key Laboratory of Cancer Prevention and Intervention, Ministry of Education, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, 310009, China
- Cancer Center, Zhejiang University, Hangzhou, Zhejiang, 310058, China
- Department of Radiation Oncology, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, 310009, China
| |
Collapse
|
|
3
|
Zhu H, Jin RU. The role of the fibroblast in Barrett's esophagus and esophageal adenocarcinoma. Curr Opin Gastroenterol 2024; 40:319-327. [PMID: 38626060 PMCID: PMC11155289 DOI: 10.1097/mog.0000000000001032] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Submit a Manuscript] [Subscribe] [Scholar Register] [Indexed: 04/18/2024]
Abstract
PURPOSE OF REVIEW Barrett's esophagus (BE) is the number one risk factor for developing esophageal adenocarcinoma (EAC), a deadly cancer with limited treatment options that has been increasing in incidence in the US. In this report, we discuss current studies on the role of mesenchyme and cancer-associated fibroblasts (CAFs) in BE and EAC, and we highlight translational prospects of targeting these cells. RECENT FINDINGS New insights through studies using single-cell RNA sequencing (sc-RNA seq) have revealed an important emerging role of the mesenchyme in developmental signaling and cancer initiation. BE and EAC share similar stromal gene expression, as functional classifications of nonepithelial cells in BE show a remarkable similarity to EAC CAFs. Several recent sc-RNA seq studies and novel organoid fibroblast co-culture systems have characterized the subgroups of fibroblasts in BE and EAC, and have shown that these cells can directly influence the epithelium to induce BE development and cancer progression. Targeting the CAFs in EAC with may be a promising novel therapeutic strategy. SUMMARY The fibroblasts in the surrounding mesenchyme may have a direct role in influencing altered epithelial plasticity during BE development and progression to EAC.
Collapse
Affiliation(s)
- Huili Zhu
- Section of Hematology/Oncology, Department of Medicine, Baylor College of Medicine, Houston, Texas, USA
| | | |
Collapse
|
|
4
|
Chen C, Liu J, Lin X, Xiang A, Ye Q, Guo J, Rui T, Xu J, Hu S. Crosstalk between cancer-associated fibroblasts and regulated cell death in tumors: insights into apoptosis, autophagy, ferroptosis, and pyroptosis. Cell Death Discov 2024; 10:189. [PMID: 38649701 PMCID: PMC11035635 DOI: 10.1038/s41420-024-01958-9] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/14/2024] [Revised: 04/10/2024] [Accepted: 04/11/2024] [Indexed: 04/25/2024] Open
Abstract
Cancer-associated fibroblasts (CAFs), the main stromal component of the tumor microenvironment (TME), play multifaceted roles in cancer progression through paracrine signaling, exosome transfer, and cell interactions. Attractively, recent evidence indicates that CAFs can modulate various forms of regulated cell death (RCD) in adjacent tumor cells, thus involving cancer proliferation, therapy resistance, and immune exclusion. Here, we present a brief introduction to CAFs and basic knowledge of RCD, including apoptosis, autophagy, ferroptosis, and pyroptosis. In addition, we further summarize the different types of RCD in tumors that are mediated by CAFs, as well as the effects of these modes of RCD on CAFs. This review will deepen our understanding of the interactions between CAFs and RCD and might offer novel therapeutic avenues for future cancer treatments.
Collapse
Affiliation(s)
- Cong Chen
- Department of Breast Surgery, Affiliated Hangzhou First People's Hospital, School of Medicine, Westlake University, Hangzhou, China
| | - Jian Liu
- Department of Breast Surgery, Affiliated Hangzhou First People's Hospital, School of Medicine, Westlake University, Hangzhou, China
| | - Xia Lin
- Department of Breast Surgery, Affiliated Hangzhou First People's Hospital, School of Medicine, Westlake University, Hangzhou, China
| | - Aizhai Xiang
- Department of Breast Surgery, Affiliated Hangzhou First People's Hospital, School of Medicine, Westlake University, Hangzhou, China
| | - Qianwei Ye
- Department of Breast Surgery, Affiliated Hangzhou First People's Hospital, School of Medicine, Westlake University, Hangzhou, China
| | - Jufeng Guo
- Department of Breast Surgery, Affiliated Hangzhou First People's Hospital, School of Medicine, Westlake University, Hangzhou, China
| | - Tao Rui
- Department of Breast Surgery, Affiliated Hangzhou First People's Hospital, School of Medicine, Westlake University, Hangzhou, China
| | - Jian Xu
- Department of Central Laboratory, Affiliated Hangzhou First People's Hospital, School of Medicine, Westlake University, Hangzhou, China
| | - Shufang Hu
- Department of Breast Surgery, Affiliated Hangzhou First People's Hospital, School of Medicine, Westlake University, Hangzhou, China.
| |
Collapse
|
|
5
|
Huang Y, Xu X, Lu Y, Sun Q, Zhang L, Shao J, Chen D, Chang Y, Sun X, Zhuo W, Zhou T. The phase separation of extracellular matrix protein matrilin-3 from cancer-associated fibroblasts contributes to gastric cancer invasion. FASEB J 2024; 38:e23406. [PMID: 38193601 DOI: 10.1096/fj.202301524r] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/27/2023] [Revised: 11/23/2023] [Accepted: 12/19/2023] [Indexed: 01/10/2024]
Abstract
Cancer-associated fibroblast (CAF) has emerged as a key contributor to the remodeling of tumor microenvironment through the expression and secretion of extracellular matrix (ECM) proteins, thereby promoting carcinogenesis. However, the precise contribution of ECM proteins from CAFs to gastric carcinogenesis remains poorly understood. In this study, we find that matrilin-3 (MATN3), an upregulated ECM protein associated with poorer prognosis in gastric cancer patients, originates from CAFs in gastric cancer tissues. Ectopic expression of MATN3 in CAFs significantly promotes the invasion of gastric cancer cells, which can be attenuated by neutralizing MATN3 with its antibody. Notably, a portion of MATN3 protein is found to form puncta in gastric cancer tissues ECM. MATN3 undergoes phase separation, which is mediated by its low complexity (LC) and coiled-coil (CC) domains. Moreover, overexpression of MATN3 deleted with either LC or CC in CAFs is unable to promote the invasion of gastric cancer cells, suggesting that LC or CC domain is required for the effect of CAF-secreted MATN3 in gastric cancer cell invasion. Additionally, orthotopic co-injection of gastric cancer cells and CAFs expressing MATN3, but not its ΔLC and ΔCC mutants, leads to enhanced gastric cancer cell invasion in mouse models. Collectively, our works suggest that MATN3 is secreted by CAFs and undergoes phase separation, which promotes gastric cancer invasion.
Collapse
Affiliation(s)
- Yuliang Huang
- Department of Cell Biology, Zhejiang University School of Medicine, Hangzhou, China
| | - Xiaoyang Xu
- Department of Cell Biology, Zhejiang University School of Medicine, Hangzhou, China
| | - Yunkun Lu
- Department of Cell Biology, Zhejiang University School of Medicine, Hangzhou, China
- Sir Run Run Shaw Hospital, Zhejiang University School of Medicine, Hangzhou, China
| | - Qiang Sun
- Center for RNA Medicine, International Institutes of Medicine and the Fourth Affiliated Hospital, Zhejiang University School of Medicine, Yiwu, China
| | - Lu Zhang
- Department of Cell Biology, Zhejiang University School of Medicine, Hangzhou, China
| | - Jiaqi Shao
- Department of Cell Biology, Zhejiang University School of Medicine, Hangzhou, China
| | - Dingwei Chen
- Department of General Surgery, Sir Run Run Shaw Hospital, Zhejiang University School of Medicine, Hangzhou, China
| | - Yongxia Chang
- Department of Cell Biology, Zhejiang University School of Medicine, Hangzhou, China
| | - Xiaoxia Sun
- Department of Cell Biology, Zhejiang University School of Medicine, Hangzhou, China
| | - Wei Zhuo
- Department of Cell Biology, Zhejiang University School of Medicine, Hangzhou, China
| | - Tianhua Zhou
- Department of Cell Biology, Zhejiang University School of Medicine, Hangzhou, China
- Center for Medical Research and Innovation in Digestive System Tumors, Ministry of Education, Hangzhou, China
- Zhejiang University Cancer Center, Hangzhou, China
| |
Collapse
|
|
6
|
Dunbar KJ, Wong KK, Rustgi AK. Cancer-Associated Fibroblasts in Esophageal Cancer. Cell Mol Gastroenterol Hepatol 2024; 17:687-695. [PMID: 38246591 PMCID: PMC10958110 DOI: 10.1016/j.jcmgh.2024.01.008] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Submit a Manuscript] [Subscribe] [Scholar Register] [Received: 11/03/2023] [Revised: 01/09/2024] [Accepted: 01/09/2024] [Indexed: 01/23/2024]
Abstract
Cancer-associated fibroblasts (CAFs), a heterogenous population, can promote cancer cell proliferation, migration, invasion, immunosuppression, and therapeutic resistance in solid tumors. These effects are mediated through secretion of cytokines and growth factors, remodeling of the extracellular matrix, and providing metabolic support for cancer cells. The presence of CAFs in esophageal carcinoma are associated with reduced overall survival and increased resistance to chemotherapy and radiotherapy; thus, identifying therapeutic vulnerabilities of CAFs is a necessity. In esophageal cancer, the mechanisms for CAF recruitment, CAF-mediated promotion of tumorigenesis, metastatic dissemination, and therapeutic resistance have yet to be fully evaluated. Here, we provide an overview of the current understanding of CAFs in esophageal cancer, namely in esophageal squamous cell carcinoma and esophageal adenocarcinoma, as well as in the preneoplastic conditions that predispose to these cancers. Interestingly, there is a discrepancy in our knowledge of CAF biology between esophageal cancer subtypes, with very few studies in esophageal adenocarcinoma, and its precursor lesion Barrett's esophagus, compared with esophageal squamous cell carcinoma. We propose that although great strides have been made, certain questions remain to which answers hopefully will emerge to have an impact on biomarker diagnostics and translational therapeutics.
Collapse
Affiliation(s)
- Karen J Dunbar
- Division of Digestive and Liver Diseases, Department of Medicine, Herbert Irving Comprehensive Cancer Center, Vagelos College of Physicians and Surgeons, Columbia University Irving Medical Center, New York, New York
| | - Kwok K Wong
- Division of Hematology-Oncology, Perlmutter Cancer Center, New York University Langone Health, New York, New York
| | - Anil K Rustgi
- Division of Digestive and Liver Diseases, Department of Medicine, Herbert Irving Comprehensive Cancer Center, Vagelos College of Physicians and Surgeons, Columbia University Irving Medical Center, New York, New York.
| |
Collapse
|
|
7
|
Belle CJ, Lonie JM, Brosda S, Barbour AP. Tumour microenvironment influences response to treatment in oesophageal adenocarcinoma. Front Immunol 2023; 14:1330635. [PMID: 38155973 PMCID: PMC10753779 DOI: 10.3389/fimmu.2023.1330635] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/31/2023] [Accepted: 11/30/2023] [Indexed: 12/30/2023] Open
Abstract
The poor treatment response of oesophageal adenocarcinoma (OAC) leads to low survival rates. Its increasing incidence makes finding more effective treatment a priority. Recent treatment improvements can be attributed to the inclusion of the tumour microenvironment (TME) and immune infiltrates in treatment decisions. OAC TME is largely immunosuppressed and reflects treatment resistance as patients with inflamed TME have better outcomes. Priming the tumour with the appropriate neoadjuvant chemoradiotherapy treatment could lead to higher immune infiltrations and higher expression of immune checkpoints, such as PD-1/PDL-1, CTLA4 or emerging new targets: LAG-3, TIM-3, TIGIT or ICOS. Multiple trials support the addition of immune checkpoint inhibitors to the current standard of care. However, results vary, supporting the need for better response biomarkers based on TME composition. This review explores what is known about OAC TME, the clinical significance of the various cell populations infiltrating it and the emerging therapeutical combination with a focus on immune checkpoints inhibitors.
Collapse
Affiliation(s)
- Clemence J. Belle
- Surgical Oncology Group, Frazer Institute, The University of Queensland, Brisbane, QLD, Australia
| | - James M. Lonie
- Surgical Oncology Group, Frazer Institute, The University of Queensland, Brisbane, QLD, Australia
| | - Sandra Brosda
- Surgical Oncology Group, Frazer Institute, The University of Queensland, Brisbane, QLD, Australia
| | - Andrew P. Barbour
- Surgical Oncology Group, Frazer Institute, The University of Queensland, Brisbane, QLD, Australia
- Department of Surgery, Princess Alexandra Hospital, Brisbane, QLD, Australia
| |
Collapse
|
|
8
|
Xue M, Tong Y, Xiong Y, Yu C. Role of cancer-associated fibroblasts in the progression, therapeutic resistance and targeted therapy of oesophageal squamous cell carcinoma. Front Oncol 2023; 13:1257266. [PMID: 37927475 PMCID: PMC10623436 DOI: 10.3389/fonc.2023.1257266] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/12/2023] [Accepted: 09/11/2023] [Indexed: 11/07/2023] Open
Abstract
Oesophageal squamous cell carcinoma (ESCC) is one of the most aggressive malignant tumours with high morbidity and mortality. Although surgery, radiotherapy and chemotherapy are common treatment options available for oesophageal cancer, the 5-year survival rate remains low after treatment. On the one hand, many oesophageal cancers are are discovered at an advanced stage and, on the other hand, treatment resistance is a major obstacle to treating locally advanced ESCC. Cancer-associated fibroblasts (CAFs), the main type of stromal cell in the tumour microenvironment, enhance tumour progression and treatment resistance and have emerged as a major focus of study on targeted therapy of oesophageal cancer.With the aim of providing potential, prospective targets for improving therapeutic efficacy, this review summarises the origin and activation of CAFs and their specific role in regulating tumour progression and treatment resistance in ESCC. We also emphasize the clinical potential and emerging trends of ESCC CAFs-targeted treatments.
Collapse
Affiliation(s)
| | | | | | - Changhua Yu
- Department of Radiotherapy, The Affiliated Huaian No.1 People’s Hospital of Nanjing Medical University, Huaian, China
| |
Collapse
|
|
9
|
Cho A, Jin W, Lee J, Shin N, Lee MS, Li L, Yang SH, Park KS, Yang CW, Kim DK, Oh YK, Lim CS, Lee JP. Periostin deficiency attenuates kidney fibrosis in diabetic nephropathy by improving pancreatic β-cell dysfunction and reducing kidney EMT. Sci Rep 2023; 13:17599. [PMID: 37845302 PMCID: PMC10579313 DOI: 10.1038/s41598-023-44177-5] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 03/26/2023] [Accepted: 10/04/2023] [Indexed: 10/18/2023] Open
Abstract
Diabetic nephropathy (DN) is associated with kidney fibrosis. A previous study revealed that periostin (POSTN) contributes to kidney fibrosis. This study examined the role of POSTN in DN. The urinary concentrations of POSTN and TNC increased according to the severity of DN in human samples. Streptozotocin (STZ) was administered after unilateral nephrectomy (UNXSTZ) to induce DN in wild-type and Postn-null mice. Four experimental groups were generated: wild-typeham (WT Sham), wild-type UNXSTZ (WT STZ), Postn-null Sham (KO Sham), and Postn-null UNXSTZ (KO STZ). After 20 weeks, the KO STZ group had lower levels of urine albumin excretion, glomerular sclerosis, and interstitial fibrosis than those of the WT STZ group. Additionally, the KO STZ group had lower expression of fibrosis markers, including TNC. The KO STZ group showed better glucose regulation than the WT STZ model. Furthermore, the KO STZ group exhibited significantly preserved pancreatic islet integrity and insulin expression. HK-2 cells were used to observe the aggravation of fibrosis caused by POSTN under TGF-β conditions. We stimulated INS-1 cells with streptozotocin and evaluated the viability of these cells. The anti-POSTN antibody treatment of INS-1 cells with streptozotocin resulted in higher cell viability than that with treatment with streptozotocin alone. The absence of POSTN in DN contributes to renal fibrosis alleviation by improving pancreatic β-cell function. Additionally, there is an association between POSTN and TNC.
Collapse
Affiliation(s)
- Ara Cho
- Translational Medicine Major, Seoul National University College of Medicine, Seoul, Republic of Korea
| | - Wencheng Jin
- Department of Internal Medicine, Seoul National University Boramae Medical Center, 20, Boramae-ro 5-gil, Dongjak-gu, Seoul, 07061, Republic of Korea
- Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea
| | - Jeonghwan Lee
- Department of Internal Medicine, Seoul National University Boramae Medical Center, 20, Boramae-ro 5-gil, Dongjak-gu, Seoul, 07061, Republic of Korea
- Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea
| | - Nayeon Shin
- Department of Internal Medicine, Seoul National University Boramae Medical Center, 20, Boramae-ro 5-gil, Dongjak-gu, Seoul, 07061, Republic of Korea
| | - Myoung Seok Lee
- Department of Radiology, Seoul National University Boramae Medical Center, Seoul, Republic of Korea
| | - Lilin Li
- Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea
- Department of Critical Care Medicine, Yanbian University Hospital, Yanji, Jilin, China
| | - Seung Hee Yang
- Biomedical Research Institute, Seoul National University Hospital, Seoul, Republic of Korea
- Kidney Research Institute, Seoul National University, Seoul, Republic of Korea
| | - Kyong Soo Park
- Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea
- Department of Internal Medicine, Seoul National University Hospital, Seoul, Republic of Korea
| | - Chul Woo Yang
- Transplantation Research Center, Department of Internal Medicine, Seoul St. Mary's Hospital, College of Medicine, The Catholic University of Korea, Seoul, Korea
| | - Dong Ki Kim
- Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea
- Department of Internal Medicine, Seoul National University Hospital, Seoul, Republic of Korea
| | - Yun Kyu Oh
- Department of Internal Medicine, Seoul National University Boramae Medical Center, 20, Boramae-ro 5-gil, Dongjak-gu, Seoul, 07061, Republic of Korea
- Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea
| | - Chun Soo Lim
- Department of Internal Medicine, Seoul National University Boramae Medical Center, 20, Boramae-ro 5-gil, Dongjak-gu, Seoul, 07061, Republic of Korea
- Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea
| | - Jung Pyo Lee
- Translational Medicine Major, Seoul National University College of Medicine, Seoul, Republic of Korea.
- Department of Internal Medicine, Seoul National University Boramae Medical Center, 20, Boramae-ro 5-gil, Dongjak-gu, Seoul, 07061, Republic of Korea.
- Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Republic of Korea.
| |
Collapse
|
|
10
|
Zhao Z, Li T, Yuan Y, Zhu Y. What is new in cancer-associated fibroblast biomarkers? Cell Commun Signal 2023; 21:96. [PMID: 37143134 PMCID: PMC10158035 DOI: 10.1186/s12964-023-01125-0] [Citation(s) in RCA: 12] [Impact Index Per Article: 12.0] [Reference Citation Analysis] [Abstract] [Key Words] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/18/2023] [Accepted: 04/05/2023] [Indexed: 05/06/2023] Open
Abstract
The tumor microenvironment is one of the important drivers of tumor development. Cancer-associated fibroblasts (CAFs) are a major component of the tumor stroma and actively participate in tumor development, invasion, metastasis, drug resistance, and other biological behaviors. CAFs are a highly heterogeneous group of cells, a reflection of the diversity of their origin, biomarkers, and functions. The diversity of CAF origin determines the complexity of CAF biomarkers, and CAF subpopulations expressing different biomarkers may play contrasting roles in tumor progression. In this review, we provide an overview of these emerging CAF biomarkers and the biological functions that they suggest, which may give a better understanding of the relationship between CAFs and tumor cells and be of great significance for breakthroughs in precision targeted therapy for tumors. Video Abstract.
Collapse
Affiliation(s)
- Zehua Zhao
- Department of Pathology, Affiliated Cancer Hospital of Dalian University of Technology (Liaoning Cancer Hospital and Institute, Cancer Hospital of China Medical University), No. 44 of Xiaoheyan Road, Dadong District, Shenyang, 110042, China
| | - Tianming Li
- Department of Pathology, Affiliated Cancer Hospital of Dalian University of Technology (Liaoning Cancer Hospital and Institute, Cancer Hospital of China Medical University), No. 44 of Xiaoheyan Road, Dadong District, Shenyang, 110042, China
| | - Yuan Yuan
- Tumor Etiology and Screening Department of Cancer Institute and General Surgery, The First Hospital of China Medical University, Shenyang, China.
- Key Laboratory of Cancer Etiology and Prevention in Liaoning Education Department, The First Hospital of China Medical University, Shenyang, China.
- Key Laboratory of GI Cancer Etiology and Prevention in Liaoning Province, The First Hospital of China Medical University, No. 155 of Nanjing Road, Heping District, Shenyang, 110001, China.
| | - Yanmei Zhu
- Department of Pathology, Affiliated Cancer Hospital of Dalian University of Technology (Liaoning Cancer Hospital and Institute, Cancer Hospital of China Medical University), No. 44 of Xiaoheyan Road, Dadong District, Shenyang, 110042, China.
| |
Collapse
|
|
11
|
Dzobo K, Dandara C. The Extracellular Matrix: Its Composition, Function, Remodeling, and Role in Tumorigenesis. Biomimetics (Basel) 2023; 8:146. [PMID: 37092398 PMCID: PMC10123695 DOI: 10.3390/biomimetics8020146] [Citation(s) in RCA: 4] [Impact Index Per Article: 4.0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/03/2023] [Revised: 03/31/2023] [Accepted: 04/03/2023] [Indexed: 04/25/2023] Open
Abstract
The extracellular matrix (ECM) is a ubiquitous member of the body and is key to the maintenance of tissue and organ integrity. Initially thought to be a bystander in many cellular processes, the extracellular matrix has been shown to have diverse components that regulate and activate many cellular processes and ultimately influence cell phenotype. Importantly, the ECM's composition, architecture, and stiffness/elasticity influence cellular phenotypes. Under normal conditions and during development, the synthesized ECM constantly undergoes degradation and remodeling processes via the action of matrix proteases that maintain tissue homeostasis. In many pathological conditions including fibrosis and cancer, ECM synthesis, remodeling, and degradation is dysregulated, causing its integrity to be altered. Both physical and chemical cues from the ECM are sensed via receptors including integrins and play key roles in driving cellular proliferation and differentiation and in the progression of various diseases such as cancers. Advances in 'omics' technologies have seen an increase in studies focusing on bidirectional cell-matrix interactions, and here, we highlight the emerging knowledge on the role played by the ECM during normal development and in pathological conditions. This review summarizes current ECM-targeted therapies that can modify ECM tumors to overcome drug resistance and better cancer treatment.
Collapse
Affiliation(s)
- Kevin Dzobo
- Medical Research Council, SA Wound Healing Unit, Hair and Skin Research Laboratory, Division of Dermatology, Department of Medicine, Groote Schuur Hospital, Faculty of Health Sciences, University of Cape Town, Anzio Road, Observatory, Cape Town 7925, South Africa
| | - Collet Dandara
- Division of Human Genetics and Institute of Infectious Disease and Molecular Medicine, Department of Pathology, Faculty of Health Sciences, University of Cape Town, Anzio Road, Observatory, Cape Town 7925, South Africa
- The South African Medical Research Council-UCT Platform for Pharmacogenomics Research and Translation, Department of Pathology, Faculty of Health Sciences, University of Cape Town, Anzio Road, Observatory, Cape Town 7925, South Africa
| |
Collapse
|
|
12
|
Ye M, Huang X, Wu Q, Liu F. Senescent Stromal Cells in the Tumor Microenvironment: Victims or Accomplices? Cancers (Basel) 2023; 15:cancers15071927. [PMID: 37046588 PMCID: PMC10093305 DOI: 10.3390/cancers15071927] [Citation(s) in RCA: 2] [Impact Index Per Article: 2.0] [Reference Citation Analysis] [Abstract] [Key Words] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/15/2023] [Revised: 03/11/2023] [Accepted: 03/21/2023] [Indexed: 04/14/2023] Open
Abstract
Cellular senescence is a unique cellular state. Senescent cells enter a non-proliferative phase, and the cell cycle is arrested. However, senescence is essentially an active cellular phenotype, with senescent cells affecting themselves and neighboring cells via autocrine and paracrine patterns. A growing body of research suggests that the dysregulation of senescent stromal cells in the microenvironment is tightly associated with the development of a variety of complex cancers. The role of senescent stromal cells in impacting the cancer cell and tumor microenvironment has also attracted the attention of researchers. In this review, we summarize the generation of senescent stromal cells in the tumor microenvironment and their specific biological functions. By concluding the signaling pathways and regulatory mechanisms by which senescent stromal cells promote tumor progression, distant metastasis, immune infiltration, and therapy resistance, this paper suggests that senescent stromal cells may serve as potential targets for drug therapy, thus providing new clues for future related research.
Collapse
Affiliation(s)
- Minghan Ye
- State Key Laboratory of Oral Diseases, National Clinical Research Center for Oral Diseases, National Center for Stomatology, West China School of Stomatology, Sichuan University, Chengdu 610065, China
| | - Xinyi Huang
- Department of Orthodontics, School and Hospital of Stomatology, Cheeloo College of Medicine, Shandong University & Shandong Key Laboratory of Oral Tissue Regeneration & Shandong Engineering Laboratory for Dental Materials and Oral Tissue Regeneration, Jinan 250100, China
| | - Qianju Wu
- Stomatological Hospital of Xiamen Medical College, Xiamen Key Laboratory of Stomatological Disease Diagnosis and Treatment, Xiamen 361008, China
- Shanghai Ninth People's Hospital, School of Medicine, Shanghai Jiao Tong University, Shanghai 200011, China
| | - Fei Liu
- State Key Laboratory of Oral Diseases, National Clinical Research Center for Oral Diseases, National Center for Stomatology, West China School of Stomatology, Sichuan University, Chengdu 610065, China
| |
Collapse
|
|
13
|
Zhang Q, Wang Y, Liu F. Cancer-associated fibroblasts: Versatile mediators in remodeling the tumor microenvironment. Cell Signal 2023; 103:110567. [PMID: 36538999 DOI: 10.1016/j.cellsig.2022.110567] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 11/12/2022] [Revised: 12/13/2022] [Accepted: 12/16/2022] [Indexed: 12/23/2022]
Abstract
Current cancer therapeutic strategies are generally not sufficient to eradicate malignancy, as cancer stroma cells contribute to tumor evasion and therapeutic resistance. Cancer-associated fibroblasts (CAFs) constitute a largely heterogeneous type of stromal cell population and are important components of the tumor microenvironment (TME). CAFs are the most abundant stromal cell type and are actively involved in tumor progression through complex mechanisms involving effects on other cell types. Research conducted in recent years has emphasized an emerging function of CAFs in the remodeling of the TME that promotes tumor progression with effects on response to treatment by various molecular mechanisms. A comprehensive mechanism of tumor-promoting activities of CAFs could facilitate the development of novel diagnostic and therapeutic approaches. In this review, the biological characterization of CAFs and the mechanisms of their effects on TME remodeling are summarized. Furthermore, we also highlight currently available therapeutic strategies targeting CAF in the context of optimizing the success of immunotherapies and briefly discuss possible future perspectives and challenges related to CAF studies.
Collapse
Affiliation(s)
- Qing Zhang
- Department of Neurosurgery, Beijing Chaoyang Hospital, Capital Medical University, Beijing 100020, China
| | - Yang Wang
- Department of Neurosurgery, Beijing Chaoyang Hospital, Capital Medical University, Beijing 100020, China.
| | - Fusheng Liu
- Brain Tumor Research Center, Beijing Neurosurgical Institute, Capital Medical University, Beijing 100070, China; Department of Neurosurgery, Beijing Tiantan Hospital Affiliated to Capital Medical University, Beijing 100070, China; Beijing Laboratory of Biomedical Materials, Beijing 100070, China.
| |
Collapse
|
|
14
|
Ishibashi Y, Mochizuki S, Horiuchi K, Tsujimoto H, Kouzu K, Kishi Y, Okada Y, Ueno H. Periostin derived from cancer-associated fibroblasts promotes esophageal squamous cell carcinoma progression via ADAM17 activation. Biochim Biophys Acta Mol Basis Dis 2023; 1869:166669. [PMID: 36813090 DOI: 10.1016/j.bbadis.2023.166669] [Citation(s) in RCA: 3] [Impact Index Per Article: 3.0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/07/2022] [Revised: 02/12/2023] [Accepted: 02/13/2023] [Indexed: 02/24/2023]
Abstract
Periostin (POSTN) is a matricellular protein that was originally identified in osteoblasts. Past studies have shown that POSTN is also preferentially expressed in cancer-associated fibroblasts (CAFs) in various types of cancer. We previously demonstrated that the increased expression of POSTN in stromal tissues is associated with an unfavorable clinical outcome in esophageal squamous cell carcinoma (ESCC) patients. In this study, we aimed to elucidate the role of POSNT in ESCC progression and its underlying molecular mechanism. We found that POSTN is predominantly produced by CAFs in ESCC tissues, and that CAFs-cultured media significantly promoted the migration, invasion, proliferation, and colony formation of ESCC cell lines in a POSTN-dependent manner. In ESCC cells, POSTN increased the phosphorylation of ERK1/2 and stimulated the expression and activity of a disintegrin and metalloproteinase 17 (ADAM17), which is critically involved in tumorigenesis and tumor progression. The effects of POSTN on ESCC cells were suppressed by interfering with the binding of POSTN to integrin αvβ3 or αvβ5 using neutralizing antibody against POSTN. Taken together, our data show that CAFs-derived POSTN stimulates ADAM17 activity through activation of the integrin αvβ3 or αvβ5-ERK1/2 pathway and thereby contributes to the progression of ESCC.
Collapse
Affiliation(s)
- Yusuke Ishibashi
- Department of Surgery, National Defense Medical College, Tokorozawa, Saitama, Japan
| | - Satsuki Mochizuki
- Department of Surgery, National Defense Medical College, Tokorozawa, Saitama, Japan.
| | - Keisuke Horiuchi
- Department of Orthopedic Surgery, National Defense Medical College, Tokorozawa, Saitama, Japan
| | - Hironori Tsujimoto
- Department of Surgery, National Defense Medical College, Tokorozawa, Saitama, Japan
| | - Keita Kouzu
- Department of Surgery, National Defense Medical College, Tokorozawa, Saitama, Japan
| | - Yoji Kishi
- Department of Orthopedic Surgery, National Defense Medical College, Tokorozawa, Saitama, Japan
| | - Yasunori Okada
- Department of Pathophysiology for Locomotive and Neoplastic Diseases, Juntendo University Graduate School of Medicine, Tokyo, Japan
| | - Hideki Ueno
- Department of Surgery, National Defense Medical College, Tokorozawa, Saitama, Japan
| |
Collapse
|
|
15
|
Lu S, Peng L, Ma F, Chai J, Hua Y, Yang W, Zhang Z. Increased Expression of POSTN Predicts Poor Prognosis: a Potential Therapeutic Target for Gastric Cancer. J Gastrointest Surg 2023; 27:233-249. [PMID: 36451060 DOI: 10.1007/s11605-022-05517-4] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Submit a Manuscript] [Subscribe] [Scholar Register] [Received: 07/23/2022] [Accepted: 10/30/2022] [Indexed: 01/20/2023]
Abstract
BACKGROUND Periostin (POSTN) is involved in many biological processes and is associated with the occurrence and development of several cancers, while its role in gastric cancer is not clear. We aimed to demonstrate the relationship between POSTN and gastric cancer based on publicly available data from The Cancer Genome Atlas (TCGA) database. METHODS POSTN expression data and corresponding clinical information were downloaded from TCGA database. We compared the expression of POSTN in gastric cancer samples and normal samples. POSTN-related differentially expressed genes (DEGs) were identified for further functional enrichment analysis. In addition, the relationships between POSTN expression and clinicopathological features and survival in patients with gastric cancer were also investigated through univariate and multivariate Cox regression analyses. Furthermore, a nomogram was constructed to predict the survival probability of gastric cancer patients. RESULTS POSTN expression in gastric cancer was significantly higher than that in normal gastric tissues (p < 0.001). High POSTN expression in gastric cancer was significantly related to poor prognostic features, including greater tumor extent (odds ratio [OR] = 1.638 for T3 and T4 vs. T1 and T2), worse histological type (OR = 0.329 for diffuse type vs. tubular type), and advanced histological grade (OR = 1.646 for grade 3 vs. grades 1 and 2) (all p < 0.05). The 118 identified DEGs were primarily enriched in pathways related to tumorigenesis and tumor progression, including the TGF-β signaling pathway, the WNT signaling pathway, and the signaling by VEGF. POSTN expression was positively correlated with the enrichment of the macrophages (r = 0.599, p < 0.001), helper T2 cells (r = 0.146, p = 0.005), and CD8 + T cells (r = 0.190, p < 0.001), but negatively correlated with the enrichment of Th17 cells (r = - 0.130, p = 0.012) and NK CD56bright cells. Kaplan-Meier survival analysis showed that high POSTN expression is associated with a short overall survival (hazard ratio [HR] = 1.54; p = 0.011). In the multivariate cox regression analysis, high POSTN expression was confirmed to be an independent predictor of poor overall survival (HR = 1.681; p = 0.017). The constructed nomogram can well predict the 1 and 3 years overall survival probability of patients with GC (0.696 [95% CI, 0.671-0.721]). CONCLUSION POSTN plays an important role in the progression and prognosis of gastric cancer, and it may serve as a useful biomarker to predict survival in gastric cancer patients.
Collapse
Affiliation(s)
- Shuaibing Lu
- Department of General Surgery, The Affiliated Cancer Hospital of Zhengzhou University & Henan Cancer Hospital, No. 127 Dongming Rd, Zhengzhou, 450008, Henan, China
| | - Liangqun Peng
- Department of General Surgery, The Affiliated Cancer Hospital of Zhengzhou University & Henan Cancer Hospital, No. 127 Dongming Rd, Zhengzhou, 450008, Henan, China
| | - Fei Ma
- Department of General Surgery, The Affiliated Cancer Hospital of Zhengzhou University & Henan Cancer Hospital, No. 127 Dongming Rd, Zhengzhou, 450008, Henan, China
| | - Junhui Chai
- Department of General Surgery, The Affiliated Cancer Hospital of Zhengzhou University & Henan Cancer Hospital, No. 127 Dongming Rd, Zhengzhou, 450008, Henan, China
| | - Yawei Hua
- Department of General Surgery, The Affiliated Cancer Hospital of Zhengzhou University & Henan Cancer Hospital, No. 127 Dongming Rd, Zhengzhou, 450008, Henan, China.
| | - Wei Yang
- Department of General Surgery, The Affiliated Cancer Hospital of Zhengzhou University & Henan Cancer Hospital, No. 127 Dongming Rd, Zhengzhou, 450008, Henan, China.
| | - Zhandong Zhang
- Department of General Surgery, The Affiliated Cancer Hospital of Zhengzhou University & Henan Cancer Hospital, No. 127 Dongming Rd, Zhengzhou, 450008, Henan, China.
| |
Collapse
|
|
16
|
Wang XY, Beeraka NM, Xue NN, Yu HM, Yang Y, Liu MX, Nikolenko VN, Liu JQ, Zhao D. Identification of a three-gene prognostic signature for radioresistant esophageal squamous cell carcinoma. World J Clin Oncol 2023; 14:13-26. [PMID: 36699628 PMCID: PMC9850665 DOI: 10.5306/wjco.v14.i1.13] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Journal Information] [Submit a Manuscript] [Subscribe] [Scholar Register] [Received: 07/25/2022] [Revised: 10/25/2022] [Accepted: 12/06/2022] [Indexed: 01/10/2023] Open
Abstract
BACKGROUND Esophageal squamous cell carcinoma (ESCC) is causing a high mortality rate due to the lack of efficient early prognosis markers and suitable therapeutic regimens. The prognostic role of genes responsible for the acquisition of radioresistance in ESCC has not been fully elucidated.
AIM To establish a prognostic model by studying gene expression patterns pertinent to radioresistance in ESCC patients.
METHODS Datasets were obtained from the Gene Expression Omnibus and The Cancer Genome Atlas databases. The edgeR, a Bioconductor package, was used to analyze mRNA expression between different groups. We screened genes specifically responsible for radioresistance to estimate overall survival. Pearson correlation analysis was performed to confirm whether the expression of those genes correlated with each other. Genes contributing to radioresistance and overall survival were assessed by the multivariate Cox regression model through the calculation of βi and risk score using the following formula: 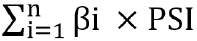 . .
RESULTS We identified three prognostic mRNAs (cathepsin S [CTSS], cluster of differentiation 180 [CD180], and SLP adapter and CSK-interacting membrane protein [SCIMP]) indicative of radioresistance. The expression of the three identified mRNAs was related to each other (r > 0.70 and P < 0.05). As to 1-year and 3-year overall survival prediction, the area under the time-dependent receiver operating characteristic curve of the signature consisting of the three mRNAs was 0.716 and 0.841, respectively. When stratifying patients based on the risk score derived from the signature, the high-risk group exhibited a higher death risk and shorter survival time than the low-risk group (P < 0.0001). Overall survival of the low-risk patients was significantly better than that of the high-risk patients (P = 0.018).
CONCLUSION We have developed a novel three-gene prognostic signature consisting of CTSS, CD180, and SCIMO for ESCC, which may facilitate the prediction of early prognosis of this malignancy.
Collapse
Affiliation(s)
- Xiao-Yan Wang
- Department of Endocrinology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
| | - Narasimha M Beeraka
- Department of Radiation Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
- Department of Human Anatomy, I. M. Sechenov First Moscow State Medical University, Moscow 119991, Russia
- Department of Pharmaceutical Chemistry, JSS College of Pharmacy, Mysuru 570015, India
| | - Nan-Nan Xue
- Department of Radiation Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
| | - Hui-Ming Yu
- Department of Radiation Oncology, Peking University Cancer Hospital & Institute, Beijing 065005, China
| | - Ya Yang
- Department of Radiation Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
| | - Mao-Xing Liu
- Key Laboratory of Carcinogenesis and Translational Research (Ministry of Education), Department of Gastrointestinal Surgery IV, Peking University Cancer Hospital & Institute, Beijing, China
| | - Vladimir N Nikolenko
- Department of Human Anatomy, I. M. Sechenov First Moscow State Medical University, Moscow 119991, Russia
- M.V. Lomonosov Moscow State University, Moscow 119991, Russia
| | - Jun-Qi Liu
- Department of Radiation Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
| | - Di Zhao
- Department of Endocrinology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou 450052, Henan Province, China
| |
Collapse
|
|
17
|
Arai J, Otoyama Y, Nozawa H, Kato N, Yoshida H. The immunological role of ADAMs in the field of gastroenterological chronic inflammatory diseases and cancers: a review. Oncogene 2023; 42:549-558. [PMID: 36572816 PMCID: PMC9937921 DOI: 10.1038/s41388-022-02583-5] [Citation(s) in RCA: 2] [Impact Index Per Article: 2.0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 10/29/2022] [Revised: 12/09/2022] [Accepted: 12/13/2022] [Indexed: 12/27/2022]
Abstract
Metalloproteinases cleave transmembrane proteins that play critical roles in inflammation and cancers. Metalloproteinases include a disintegrin and metalloprotease (ADAM), which we previously examined using a fluorescence assay system, and described their association with resistance to systemic therapy in cancer patients. There are also many reports on the relation between ADAM expression and the prognosis of patients with gastroenterological chronic inflammatory diseases and cancers. Inhibiting their immunomodulating activity in chronic inflammation restores innate immunity and potentially prevents the development of various cancers. Among the numerous critical immune system-related molecules, we focus on major histocompatibility complex class I polypeptide-related sequence A (MICA), MICB, intracellular adhesion molecule (ICAM)-1, TNF-α, IL-6 receptor (IL-6R), and Notch. This review summarizes our current understanding of the role of ADAMs in gastroenterological diseases with regard to the immune system. Several Food and Drug Administration (FDA)-approved inhibitors of ADAMs have been identified, and potential therapies for targeting ADAMs in the treatment of chronic inflammatory diseases and cancers are discussed. Some ongoing clinical trials for cancers targeting ADAMs are also introduced.
Collapse
Affiliation(s)
- Jun Arai
- Division of Gastroenterology, Department of Medicine, Showa University School of Medicine, Tokyo, Japan.
| | - Yumi Otoyama
- grid.410714.70000 0000 8864 3422Division of Gastroenterology, Department of Medicine, Showa University School of Medicine, Tokyo, Japan
| | - Hisako Nozawa
- grid.410714.70000 0000 8864 3422Division of Gastroenterology, Department of Medicine, Showa University School of Medicine, Tokyo, Japan
| | - Naoya Kato
- grid.136304.30000 0004 0370 1101Department of Gastroenterology, Graduate School of Medicine, Chiba University, Chiba, Japan
| | - Hitoshi Yoshida
- grid.410714.70000 0000 8864 3422Division of Gastroenterology, Department of Medicine, Showa University School of Medicine, Tokyo, Japan
| |
Collapse
|
|
18
|
Mellone M, Piotrowska K, Venturi G, James L, Bzura A, Lopez MA, James S, Wang C, Ellis MJ, Hanley CJ, Buckingham JF, Cox KL, Hughes G, Valge-Archer V, King EV, Beers SA, Jaquet V, Jones GD, Savelyeva N, Sayan E, Parsons JL, Durant S, Thomas GJ. ATM Regulates Differentiation of Myofibroblastic Cancer-Associated Fibroblasts and Can Be Targeted to Overcome Immunotherapy Resistance. Cancer Res 2022; 82:4571-4585. [PMID: 36353752 PMCID: PMC9755965 DOI: 10.1158/0008-5472.can-22-0435] [Citation(s) in RCA: 1] [Impact Index Per Article: 0.5] [Reference Citation Analysis] [Abstract] [MESH Headings] [Grants] [Track Full Text] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/07/2022] [Revised: 07/28/2022] [Accepted: 09/21/2022] [Indexed: 11/11/2022]
Abstract
Myofibroblastic cancer-associated fibroblast (myoCAF)-rich tumors generally contain few T cells and respond poorly to immune-checkpoint blockade. Although myoCAFs are associated with poor outcome in most solid tumors, the molecular mechanisms regulating myoCAF accumulation remain unclear, limiting the potential for therapeutic intervention. Here, we identify ataxia-telangiectasia mutated (ATM) as a central regulator of the myoCAF phenotype. Differentiating myofibroblasts in vitro and myoCAFs cultured ex vivo display activated ATM signaling, and targeting ATM genetically or pharmacologically could suppress and reverse differentiation. ATM activation was regulated by the reactive oxygen species-producing enzyme NOX4, both through DNA damage and increased oxidative stress. Targeting fibroblast ATM in vivo suppressed myoCAF-rich tumor growth, promoted intratumoral CD8 T-cell infiltration, and potentiated the response to anti-PD-1 blockade and antitumor vaccination. This work identifies a novel pathway regulating myoCAF differentiation and provides a rationale for using ATM inhibitors to overcome CAF-mediated immunotherapy resistance. SIGNIFICANCE ATM signaling supports the differentiation of myoCAFs to suppress T-cell infiltration and antitumor immunity, supporting the potential clinical use of ATM inhibitors in combination with checkpoint inhibition in myoCAF-rich, immune-cold tumors.
Collapse
Affiliation(s)
- Massimiliano Mellone
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Klaudia Piotrowska
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Giulia Venturi
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Lija James
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Aleksandra Bzura
- Department of Genetics and Genome Biology, Cancer Research Centre, University of Leicester, Leicester, United Kingdom
| | - Maria A. Lopez
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Sonya James
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Chuan Wang
- Department of Molecular and Clinical Cancer Medicine, Cancer Research Centre, University of Liverpool, Liverpool, United Kingdom
| | - Matthew J. Ellis
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Christopher J. Hanley
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Josephine F. Buckingham
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Kerry L. Cox
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Gareth Hughes
- Bioscience, Oncology Innovative Medicines and Early Development (IMED) Biotech Unit, AstraZeneca, Cambridge, United Kingdom
| | - Viia Valge-Archer
- Bioscience, Oncology Innovative Medicines and Early Development (IMED) Biotech Unit, AstraZeneca, Cambridge, United Kingdom
| | - Emma V. King
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Stephen A. Beers
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Vincent Jaquet
- Department of Pathology and Immunology, Centre Médical Universitaire, Genève, Switzerland
| | - George D.D. Jones
- Department of Genetics and Genome Biology, Cancer Research Centre, University of Leicester, Leicester, United Kingdom
| | - Natalia Savelyeva
- Department of Molecular and Clinical Cancer Medicine, Cancer Research Centre, University of Liverpool, Liverpool, United Kingdom
| | - Emre Sayan
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| | - Jason L. Parsons
- Department of Molecular and Clinical Cancer Medicine, Cancer Research Centre, University of Liverpool, Liverpool, United Kingdom
| | - Stephen Durant
- Bioscience, Oncology Innovative Medicines and Early Development (IMED) Biotech Unit, AstraZeneca, Cambridge, United Kingdom
| | - Gareth J. Thomas
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton, United Kingdom
| |
Collapse
|
|
19
|
Jenkins BH, Buckingham JF, Hanley CJ, Thomas GJ. Targeting cancer-associated fibroblasts: Challenges, opportunities and future directions. Pharmacol Ther 2022; 240:108231. [PMID: 35718294 DOI: 10.1016/j.pharmthera.2022.108231] [Citation(s) in RCA: 23] [Impact Index Per Article: 11.5] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 04/07/2022] [Revised: 06/08/2022] [Accepted: 06/13/2022] [Indexed: 02/06/2023]
Abstract
Cancer-associated fibroblasts (CAFs) are a common cell in the tumour microenvironment with diverse tumour-promoting functions. Their presence in tumours is commonly associated with poor prognosis making them attractive therapeutic targets, particularly in the context of immunotherapy where CAFs have been shown to promote resistance to checkpoint blockade. Previous attempts to inhibit CAFs clinically have not been successful, however, in part due to a lack of understanding of CAF heterogeneity and function, with some fibroblast populations potentially being tumour suppressive. Recent single-cell transcriptomic studies have advanced our understanding of fibroblast phenotypes in normal tissues and cancers, allowing for a more precise characterisation of CAF subsets and providing opportunities to develop new therapies. Here we review recent advances in the field, focusing on the evolving area of therapeutic CAF targeting.
Collapse
Affiliation(s)
- Benjamin H Jenkins
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, UK
| | | | | | - Gareth J Thomas
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, UK.
| |
Collapse
|
|
20
|
Neuzillet C, Nicolle R, Raffenne J, Tijeras‐Raballand A, Brunel A, Astorgues‐Xerri L, Vacher S, Arbateraz F, Fanjul M, Hilmi M, Samain R, Klein C, Perraud A, Rebours V, Mathonnet M, Bièche I, Kocher H, Cros J, Bousquet C. Periostin- and podoplanin-positive cancer-associated fibroblast subtypes cooperate to shape the inflamed tumor microenvironment in aggressive pancreatic adenocarcinoma. J Pathol 2022; 258:408-425. [PMID: 36102377 PMCID: PMC9828775 DOI: 10.1002/path.6011] [Citation(s) in RCA: 17] [Impact Index Per Article: 8.5] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 04/18/2022] [Revised: 08/08/2022] [Accepted: 09/10/2022] [Indexed: 01/19/2023]
Abstract
Cancer-associated fibroblasts (CAFs) are orchestrators of the pancreatic ductal adenocarcinoma (PDAC) microenvironment. Previously we described four CAF subtypes with specific molecular and functional features. Here, we have refined our CAF subtype signatures using RNAseq and immunostaining with the goal of defining bioinformatically the phenotypic stromal and tumor epithelial states associated with CAF diversity. We used primary CAF cultures grown from patient PDAC tumors, human data sets (in-house and public, including single-cell analyses), genetically engineered mouse PDAC tissues, and patient-derived xenografts (PDX) grown in mice. We found that CAF subtype RNAseq signatures correlated with immunostaining. Tumors rich in periostin-positive CAFs were significantly associated with shorter overall survival of patients. Periostin-positive CAFs were characterized by high proliferation and protein synthesis rates and low α-smooth muscle actin expression and were found in peri-/pre-tumoral areas. They were associated with highly cellular tumors and with macrophage infiltrates. Podoplanin-positive CAFs were associated with immune-related signatures and recruitment of dendritic cells. Importantly, we showed that the combination of periostin-positive CAFs and podoplanin-positive CAFs was associated with specific tumor microenvironment features in terms of stromal abundance and immune cell infiltrates. Podoplanin-positive CAFs identified an inflammatory CAF (iCAF)-like subset, whereas periostin-positive CAFs were not correlated with the published myofibroblastic CAF (myCAF)/iCAF classification. Taken together, these results suggest that a periostin-positive CAF is an early, activated CAF, associated with aggressive tumors, whereas a podoplanin-positive CAF is associated with an immune-related phenotype. These two subpopulations cooperate to define specific tumor microenvironment and patient prognosis and are of putative interest for future therapeutic stratification of patients. © 2022 The Authors. The Journal of Pathology published by John Wiley & Sons Ltd on behalf of The Pathological Society of Great Britain and Ireland.
Collapse
Affiliation(s)
- Cindy Neuzillet
- Department of Medical Oncology, Institut CurieUniversité Versailles Saint‐Quentin, Paris SaclaySaint‐CloudFrance,UMR144, Institut CurieParisFrance
| | - Rémy Nicolle
- INSERM U1149, Centre de Recherche sur l'InflammationParisFrance
| | - Jérôme Raffenne
- INSERM UMR‐1037, Cancer Research Center of Toulouse (CRCT), Team ‘labellisée Ligue Contre le Cancer’University of ToulouseToulouseFrance
| | | | - Alexia Brunel
- INSERM UMR‐1037, Cancer Research Center of Toulouse (CRCT), Team ‘labellisée Ligue Contre le Cancer’University of ToulouseToulouseFrance
| | | | - Sophie Vacher
- Department of GeneticsInstitut Curie, PSL Research UniversityParisFrance
| | - Floriane Arbateraz
- Centre d'Histologie Imagerie et Cytométrie (CHIC), U1138 Centre de Recherche des Cordeliers (CRC)ParisFrance
| | - Marjorie Fanjul
- INSERM UMR‐1037, Cancer Research Center of Toulouse (CRCT), Team ‘labellisée Ligue Contre le Cancer’University of ToulouseToulouseFrance
| | - Marc Hilmi
- Department of Medical Oncology, Institut CurieUniversité Versailles Saint‐Quentin, Paris SaclaySaint‐CloudFrance
| | - Rémi Samain
- INSERM UMR‐1037, Cancer Research Center of Toulouse (CRCT), Team ‘labellisée Ligue Contre le Cancer’University of ToulouseToulouseFrance
| | - Christophe Klein
- Centre d'Histologie Imagerie et Cytométrie (CHIC), U1138 Centre de Recherche des Cordeliers (CRC)ParisFrance
| | - Aurélie Perraud
- Department of Digestive SurgeryUniversity Hospital of LimogesLimogesFrance,INSERM UMLR‐1308University of LimogesLimogesFrance
| | - Vinciane Rebours
- INSERM U1149, Centre de Recherche sur l'InflammationParisFrance,Department of PancreatologyBeaujon Hospital (APHP)Clichy‐La‐GarenneFrance
| | - Muriel Mathonnet
- Department of Digestive SurgeryUniversity Hospital of LimogesLimogesFrance,INSERM UMLR‐1308University of LimogesLimogesFrance
| | - Ivan Bièche
- Department of GeneticsInstitut Curie, PSL Research UniversityParisFrance
| | - Hemant Kocher
- Centre for Tumour Biology, Barts Cancer Institute ‐ a CR‐UK Centre of ExcellenceQueen Mary University of LondonLondonUK
| | - Jérôme Cros
- INSERM U1149, Centre de Recherche sur l'InflammationParisFrance,Department of Pathology, Beaujon Hospital (APHP)Université de ParisParisFrance
| | - Corinne Bousquet
- INSERM UMR‐1037, Cancer Research Center of Toulouse (CRCT), Team ‘labellisée Ligue Contre le Cancer’University of ToulouseToulouseFrance
| |
Collapse
|
|
21
|
Sun J, Yang M, Zhao W, Wang F, Yang L, Tan C, Hu T, Zhu H, Zhao G. Research progress on the relationship between the TOR signaling pathway regulator, epigenetics, and tumor development. Front Genet 2022; 13:1006936. [PMID: 36212146 PMCID: PMC9539685 DOI: 10.3389/fgene.2022.1006936] [Citation(s) in RCA: 2] [Impact Index Per Article: 1.0] [Reference Citation Analysis] [Abstract] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/29/2022] [Accepted: 08/31/2022] [Indexed: 11/16/2022] Open
Abstract
Almost all cellular activities depend on protein folding, signaling complex assembly/disassembly, and epigenetic regulation. One of the most important regulatory mechanisms responsible for controlling these cellular processes is dynamic protein phosphorylation/dephosphorylation. Alterations in phosphorylation networks have major consequences in the form of disorders, including cancer. Many signaling cascades, including the target of rapamycin (TOR) signaling, are important participants in the cell cycle, and dysregulation in their phosphorylation/dephosphorylation status has been linked to malignancies. As a TOR signaling regulator, protein phosphatase 2A (PP2A) is responsible for most of the phosphatase activities inside the cells. On the other hand, TOR signaling pathway regulator (TIPRL) is an essential PP2A inhibitory protein. Many other physiological roles have also been suggested for TIPRL, such as modulation of TOR pathways, apoptosis, and cell proliferation. It is also reported that TIPRL was increased in various carcinomas, including non-small-cell lung carcinoma (NSCLC) and hepatocellular carcinomas (HCC). Considering the function of PP2A as a tumor suppressor and also the effect of the TIPRL/PP2A axis on apoptosis and proliferation of cancer cells, this review aims to provide a complete view of the role of TIPRL in cancer development in addition to describing TIPRL/PP2A axis and its epigenetic regulation.
Collapse
Affiliation(s)
- Jiaen Sun
- School of Medicine, Ningbo University, Ningbo, Zhejiang, China
- Department of Thoracic Surgery, Hwa Mei Hospital, University of Chinese Academy of Sciences, Ningbo, Zhejiang, China
| | - Minglei Yang
- School of Medicine, Ningbo University, Ningbo, Zhejiang, China
- Department of Thoracic Surgery, Hwa Mei Hospital, University of Chinese Academy of Sciences, Ningbo, Zhejiang, China
| | - Weidi Zhao
- School of Medicine, Ningbo University, Ningbo, Zhejiang, China
- Department of Thoracic Surgery, Hwa Mei Hospital, University of Chinese Academy of Sciences, Ningbo, Zhejiang, China
| | - Fajiu Wang
- Department of Thoracic Surgery, Hwa Mei Hospital, University of Chinese Academy of Sciences, Ningbo, Zhejiang, China
| | - Liangwei Yang
- Department of Thoracic Surgery, Hwa Mei Hospital, University of Chinese Academy of Sciences, Ningbo, Zhejiang, China
| | - Chuntao Tan
- Department of Cardiac and Vascular Surgery, Hwa Mei Hospital, University of Chinese Academy of Sciences, Ningbo, Zhejiang, China
| | - Tianjun Hu
- Department of Thoracic Surgery, Hwa Mei Hospital, University of Chinese Academy of Sciences, Ningbo, Zhejiang, China
| | - Huangkai Zhu
- School of Medicine, Ningbo University, Ningbo, Zhejiang, China
- Department of Thoracic Surgery, Hwa Mei Hospital, University of Chinese Academy of Sciences, Ningbo, Zhejiang, China
- *Correspondence: Huangkai Zhu, ; Guofang Zhao,
| | - Guofang Zhao
- School of Medicine, Ningbo University, Ningbo, Zhejiang, China
- Department of Thoracic Surgery, Hwa Mei Hospital, University of Chinese Academy of Sciences, Ningbo, Zhejiang, China
- *Correspondence: Huangkai Zhu, ; Guofang Zhao,
| |
Collapse
|
|
22
|
Li J, Hou W, Yang Y, Deng Q, Fu H, Yin Y, Duan K, Feng B, Guo T, Weng J. Micro/nano-topography promotes osteogenic differentiation of bone marrow stem cells by regulating periostin expression. Colloids Surf B Biointerfaces 2022; 218:112700. [PMID: 35907353 DOI: 10.1016/j.colsurfb.2022.112700] [Citation(s) in RCA: 6] [Impact Index Per Article: 3.0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 11/24/2021] [Revised: 06/07/2022] [Accepted: 07/11/2022] [Indexed: 12/18/2022]
Abstract
Micro/nano-topography (MNT) is an important factor affecting cell response. Earlier studies using titania (TiO2) nanotube as a model of MNT found that they mediated the differentiation of BMSCs into osteoblasts, but the mechanisms are not fully understood. Surprisingly, Periostin (Postn), a secreted protein involved in extracellular matrix (ECM) construction and promoting osteogenic differentiation of bone marrow stem cells (BMSCs), was previously observed to significantly up-regulated on TiO2 nanotube. We proposed that Postn may act as a MNT signal transduction role. In this study, we investigated the effect of MNT on Postn, and the influence of Postn on osteogenic differentiation-related genes through focal adhesion and downstream signals. It was found that, titanium (Ti) plates carrying TiO2 nanotubes with diameters of ∼100 nm (TNT-100) significantly up-regulated the expression of Postn compared with flat Ti. Furthermore, Postn activated the downstream focal adhesion kinase (FAK) signal pathway and β-catenin into the nucleus by interacting with integrin αV. Surprisingly, TNT-100 up-regulated the transcription level of Wnt3a, which was independent of the up-regulation of Postn. This new Postn signaling pathway may provide more insights into the signal transduction mechanism of MNT and development of biomaterials with improved osteogenic properties.
Collapse
Affiliation(s)
- Jinsheng Li
- School of Materials Science & Engineering, Southwest Jiaotong University, Chengdu 610031, China
| | - Wenqing Hou
- College of Medicine, Southwest Jiaotong University, Chengdu 610031, China
| | - Yali Yang
- School of Life Science and Engineering, Southwest Jiaotong University, Chengdu 610031, China
| | - Qing Deng
- College of Medicine, Southwest Jiaotong University, Chengdu 610031, China
| | - Hong Fu
- College of Medicine, Southwest Jiaotong University, Chengdu 610031, China
| | - Yiran Yin
- Sichuan Provincial Lab of Orthopaedic Engineering, Department of Bone and Joint Surgery, Affiliated Hospital of Southwest Medical University, Luzhou 646000, China
| | - Ke Duan
- Sichuan Provincial Lab of Orthopaedic Engineering, Department of Bone and Joint Surgery, Affiliated Hospital of Southwest Medical University, Luzhou 646000, China
| | - Bo Feng
- School of Materials Science & Engineering, Southwest Jiaotong University, Chengdu 610031, China
| | - Tailin Guo
- College of Medicine, Southwest Jiaotong University, Chengdu 610031, China.
| | - Jie Weng
- School of Materials Science & Engineering, Southwest Jiaotong University, Chengdu 610031, China; College of Medicine, Southwest Jiaotong University, Chengdu 610031, China.
| |
Collapse
|
|
23
|
Sharpe BP, Hayden A, Manousopoulou A, Cowie A, Walker RC, Harrington J, Izadi F, Breininger SP, Gibson J, Pickering O, Jaynes E, Kyle E, Saunders JH, Parsons SL, Ritchie AA, Clarke PA, Collier P, Mongan NP, Bates DO, Yacqub-Usman K, Garbis SD, Walters Z, Rose-Zerilli M, Grabowska AM, Underwood TJ. Phosphodiesterase type 5 inhibitors enhance chemotherapy in preclinical models of esophageal adenocarcinoma by targeting cancer-associated fibroblasts. Cell Rep Med 2022; 3:100541. [PMID: 35732148 PMCID: PMC9244979 DOI: 10.1016/j.xcrm.2022.100541] [Citation(s) in RCA: 1] [Impact Index Per Article: 0.5] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 09/14/2021] [Revised: 12/14/2021] [Accepted: 01/28/2022] [Indexed: 12/03/2022]
Abstract
The chemotherapy resistance of esophageal adenocarcinomas (EACs) is underpinned by cancer cell extrinsic mechanisms of the tumor microenvironment (TME). We demonstrate that, by targeting the tumor-promoting functions of the predominant TME cell type, cancer-associated fibroblasts (CAFs) with phosphodiesterase type 5 inhibitors (PDE5i), we can enhance the efficacy of standard-of-care chemotherapy. In ex vivo conditions, PDE5i prevent the transdifferentiation of normal fibroblasts to CAF and abolish the tumor-promoting function of established EAC CAFs. Using shotgun proteomics and single-cell RNA-seq, we reveal PDE5i-specific regulation of pathways related to fibroblast activation and tumor promotion. Finally, we confirm the efficacy of PDE5i in combination with chemotherapy in close-to-patient and in vivo PDX-based model systems. These findings demonstrate that CAFs drive chemotherapy resistance in EACs and can be targeted by repurposing PDE5i, a safe and well-tolerated class of drug administered to millions of patients world-wide to treat erectile dysfunction.
Collapse
Affiliation(s)
- Benjamin P Sharpe
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK
| | - Annette Hayden
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK
| | | | - Andrew Cowie
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK
| | - Robert C Walker
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK
| | - Jack Harrington
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK
| | - Fereshteh Izadi
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK; Centre for NanoHealth, Swansea University Medical School, Singleton Campus, Swansea SA2 8PP, UK
| | - Stella P Breininger
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK
| | - Jane Gibson
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK
| | - Oliver Pickering
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK
| | - Eleanor Jaynes
- University Hospital Southampton NHS Foundation Trust, Southampton SO16 6YD, UK
| | - Ewan Kyle
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK
| | - John H Saunders
- Ex Vivo Cancer Pharmacology Centre of Excellence, School of Medicine, Biodiscovery Institute, University of Nottingham, Nottingham NG7 2RD, UK; Salford Royal NHS Foundation Trust, Salford M6 8HD, UK
| | - Simon L Parsons
- Ex Vivo Cancer Pharmacology Centre of Excellence, School of Medicine, Biodiscovery Institute, University of Nottingham, Nottingham NG7 2RD, UK; Nottingham University Hospitals NHS Trust, Hucknall Road, Nottingham NG5 1PB, UK
| | - Alison A Ritchie
- Ex Vivo Cancer Pharmacology Centre of Excellence, School of Medicine, Biodiscovery Institute, University of Nottingham, Nottingham NG7 2RD, UK
| | - Philip A Clarke
- Ex Vivo Cancer Pharmacology Centre of Excellence, School of Medicine, Biodiscovery Institute, University of Nottingham, Nottingham NG7 2RD, UK
| | - Pamela Collier
- Ex Vivo Cancer Pharmacology Centre of Excellence, School of Medicine, Biodiscovery Institute, University of Nottingham, Nottingham NG7 2RD, UK
| | - Nigel P Mongan
- Department of Pharmacology, Weill Cornell Medicine, New York, NY 10065, USA; Biodiscovery Institute, School of Veterinary Medicine and Science, University of Nottingham, Nottingham NG5 1PB, UK
| | - David O Bates
- Ex Vivo Cancer Pharmacology Centre of Excellence, School of Medicine, Biodiscovery Institute, University of Nottingham, Nottingham NG7 2RD, UK
| | - Kiren Yacqub-Usman
- Ex Vivo Cancer Pharmacology Centre of Excellence, School of Medicine, Biodiscovery Institute, University of Nottingham, Nottingham NG7 2RD, UK
| | | | - Zoë Walters
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK
| | - Matthew Rose-Zerilli
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK
| | - Anna M Grabowska
- Ex Vivo Cancer Pharmacology Centre of Excellence, School of Medicine, Biodiscovery Institute, University of Nottingham, Nottingham NG7 2RD, UK
| | - Timothy J Underwood
- School of Cancer Sciences, Faculty of Medicine, Room CS B2, MP824, Somers Cancer Research Building, University Hospital Southampton, Tremona Road, Southampton SO16 6YD, UK.
| |
Collapse
|
|
24
|
Tinsley SL, Allen-Petersen BL. PP2A and cancer epigenetics: a therapeutic opportunity waiting to happen. NAR Cancer 2022; 4:zcac002. [PMID: 35118387 PMCID: PMC8807117 DOI: 10.1093/narcan/zcac002] [Citation(s) in RCA: 5] [Impact Index Per Article: 2.5] [Reference Citation Analysis] [Abstract] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 09/07/2021] [Revised: 12/08/2021] [Accepted: 01/10/2022] [Indexed: 12/13/2022] Open
Abstract
The epigenetic state of chromatin is altered by regulators which influence gene expression in response to environmental stimuli. While several post-translational modifications contribute to chromatin accessibility and transcriptional programs, our understanding of the role that specific phosphorylation sites play is limited. In cancer, kinases and phosphatases are commonly deregulated resulting in increased oncogenic signaling and loss of epigenetic regulation. Aberrant epigenetic states are known to promote cellular plasticity and the development of therapeutic resistance in many cancer types, highlighting the importance of these mechanisms to cancer cell phenotypes. Protein Phosphatase 2A (PP2A) is a heterotrimeric holoenzyme that targets a diverse array of cellular proteins. The composition of the PP2A complex influences its cellular targets and activity. For this reason, PP2A can be tumor suppressive or oncogenic depending on cellular context. Understanding the nuances of PP2A regulation and its effect on epigenetic alterations can lead to new therapeutic avenues that afford more specificity and contribute to the growth of personalized medicine in the oncology field. In this review, we summarize the known PP2A-regulated substrates and potential phosphorylation sites that contribute to cancer cell epigenetics and possible strategies to therapeutically leverage this phosphatase to suppress tumor growth.
Collapse
Affiliation(s)
- Samantha L Tinsley
- Department of Biological Sciences, Purdue University, West Lafayette, IN 47907, USA
| | | |
Collapse
|
|
25
|
Hsiao Y, Chi J, Li C, Chen L, Chen Y, Liang H, Lo Y, Hong J, Chuu C, Hung L, Du J, Chang W, Wang J. Disruption of the pentraxin 3/CD44 interaction as an efficient therapy for triple-negative breast cancers. Clin Transl Med 2022; 12:e724. [PMID: 35090088 PMCID: PMC8797470 DOI: 10.1002/ctm2.724] [Citation(s) in RCA: 15] [Impact Index Per Article: 7.5] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 12/08/2020] [Revised: 01/13/2022] [Accepted: 01/17/2022] [Indexed: 12/29/2022] Open
Abstract
Due to the heterogeneity and high frequency of genome mutations in cancer cells, targeting vital protumour factors found in stromal cells in the tumour microenvironment may represent an ideal strategy in cancer therapy. However, the regulation and mechanisms of potential targetable therapeutic candidates need to be investigated. An in vivo study demonstrated that loss of pentraxin 3 (PTX3) in stromal cells significantly decreased the metastasis and growth of cancer cells. Clinically, our results indicate that stromal PTX3 expression correlates with adverse prognostic features and is associated with worse survival outcomes in triple-negative breast cancer (TNBC). We also found that transforming growth factor beta 1 (TGF-β1) induces PTX3 expression by activating the transcription factor CCAAT/enhancer binding protein delta (CEBPD) in stromal fibroblasts. Following PTX3 stimulation, CD44, a PTX3 receptor, activates the downstream ERK1/2, AKT and NF-κB pathways to specifically contribute to the metastasis/invasion and stemness of TNBC MDA-MB-231 cells. Two types of PTX3 inhibitors were developed to disrupt the PTX3/CD44 interaction and they showed a significant effect on attenuating growth and restricting the metastasis/invasion of MDA-MB-231 cells, suggesting that targeting the PTX3/CD44 interaction could be a new strategy for future TNBC therapies.
Collapse
Affiliation(s)
- Yu‐Wei Hsiao
- Department of Biotechnology and Bioindustry Sciences, College of Bioscience and BiotechnologyNational Cheng Kung UniversityTainanTaiwan R. O. C.
| | - Jhih‐Ying Chi
- Department of Biotechnology and Bioindustry Sciences, College of Bioscience and BiotechnologyNational Cheng Kung UniversityTainanTaiwan R. O. C.
| | - Chien‐Feng Li
- Department of PathologyChi‐Mei Medical CenterTainanTaiwan R. O. C.
| | - Lei‐Yi Chen
- Department of Biotechnology and Bioindustry Sciences, College of Bioscience and BiotechnologyNational Cheng Kung UniversityTainanTaiwan R. O. C.
| | - Yi‐Ting Chen
- Department of Biotechnology and Bioindustry Sciences, College of Bioscience and BiotechnologyNational Cheng Kung UniversityTainanTaiwan R. O. C.
| | - Hsin‐Yin Liang
- Department of Biotechnology and Bioindustry Sciences, College of Bioscience and BiotechnologyNational Cheng Kung UniversityTainanTaiwan R. O. C.
| | - Yu‐Chih Lo
- Department of Biotechnology and Bioindustry Sciences, College of Bioscience and BiotechnologyNational Cheng Kung UniversityTainanTaiwan R. O. C.
| | - Jhen‐Yi Hong
- Department of Biotechnology and Bioindustry Sciences, College of Bioscience and BiotechnologyNational Cheng Kung UniversityTainanTaiwan R. O. C.
| | - Chin‐Pin Chuu
- Institute of Cellular and System MedicineNational Health Research InstitutesMiaoli CountyTaiwan R. O. C.
| | - Liang‐Yi Hung
- Department of Biotechnology and Bioindustry Sciences, College of Bioscience and BiotechnologyNational Cheng Kung UniversityTainanTaiwan R. O. C.
| | - Jyun‐Yi Du
- Department of Biotechnology and Bioindustry Sciences, College of Bioscience and BiotechnologyNational Cheng Kung UniversityTainanTaiwan R. O. C.
| | - Wen‐Chang Chang
- Graduate Institute of Medical Sciences, College of MedicineTaipei Medical UniversityTaipeiTaiwan R. O. C.
| | - Ju‐Ming Wang
- Department of Biotechnology and Bioindustry Sciences, College of Bioscience and BiotechnologyNational Cheng Kung UniversityTainanTaiwan R. O. C.
- Graduate Institute of Medical Sciences, College of MedicineTaipei Medical UniversityTaipeiTaiwan R. O. C.
- International Research Center for Wound Repair and RegenerationNational Cheng Kung UniversityTainanTaiwan R. O. C.
- Department of Physiology, College of MedicineNational Cheng Kung UniversityTainanTaiwan R. O. C.
- Graduate Institute of Medicine, College of MedicineKaohsiung Medical UniversityKaohsiungTaiwan R. O. C.
| |
Collapse
|
|
26
|
Mu J, Gao S, Yang J, Wu F, Zhou H. Fundamental and Clinical Applications of Materials Based on Cancer-Associated Fibroblasts in Cancers. Int J Mol Sci 2021; 22:11671. [PMID: 34769102 PMCID: PMC8583912 DOI: 10.3390/ijms222111671] [Citation(s) in RCA: 1] [Impact Index Per Article: 0.3] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 09/30/2021] [Revised: 10/21/2021] [Accepted: 10/26/2021] [Indexed: 02/05/2023] Open
Abstract
Cancer stromal cells play a role in promoting tumor relapse and therapeutic resistance. Therefore, the current treatment paradigms for cancers are usually insufficient to eradicate cancer cells, and anti-cancer therapeutic strategies targeting stromal cells have been developed. Cancer-associated fibroblasts (CAFs) are perpetually activated fibroblasts in the tumor stroma. CAFs are the most abundant and highly heterogeneous stromal cells, and they are critically involved in cancer occurrence and progression. These effects are due to their various roles in the remodeling of the extracellular matrix, maintenance of cancer stemness, modulation of tumor metabolism, and promotion of therapy resistance. Recently, biomaterials and nanomaterials based on CAFs have been increasingly developed to perform gene or protein expression analysis, three-dimensional (3D) co-cultivation, and targeted drug delivery in cancer treatment. In this review, we systematically summarize the current research to fully understand the relevant materials and their functional diversity in CAFs, and we highlight the potential clinical applications of CAFs-oriented biomaterials and nanomaterials in anti-cancer therapy.
Collapse
Affiliation(s)
- Jingtian Mu
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, Frontier Innovation Center for Dental Medicine Plus, West China Hospital of Stomatology, Sichuan University, Chengdu 610041, China; (J.M.); (J.Y.)
| | - Shengtao Gao
- State Key Laboratory of Oral Diseases, West China College of Stomatology, Sichuan University, Chengdu 610041, China;
| | - Jin Yang
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, Frontier Innovation Center for Dental Medicine Plus, West China Hospital of Stomatology, Sichuan University, Chengdu 610041, China; (J.M.); (J.Y.)
| | - Fanglong Wu
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, Frontier Innovation Center for Dental Medicine Plus, West China Hospital of Stomatology, Sichuan University, Chengdu 610041, China; (J.M.); (J.Y.)
| | - Hongmei Zhou
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, Frontier Innovation Center for Dental Medicine Plus, West China Hospital of Stomatology, Sichuan University, Chengdu 610041, China; (J.M.); (J.Y.)
| |
Collapse
|
|
27
|
Takahashi M, Kobayashi H, Mizutani Y, Hara A, Iida T, Miyai Y, Asai N, Enomoto A. Roles of the Mesenchymal Stromal/Stem Cell Marker Meflin/Islr in Cancer Fibrosis. Front Cell Dev Biol 2021; 9:749924. [PMID: 34676218 PMCID: PMC8523999 DOI: 10.3389/fcell.2021.749924] [Citation(s) in RCA: 28] [Impact Index Per Article: 9.3] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/30/2021] [Accepted: 09/06/2021] [Indexed: 01/03/2023] Open
Abstract
Fibroblasts synthesise the extracellular matrix (ECM) such as collagen and elastin, the excessive accumulation of which can lead to fibrosis and organ dysfunction under pathological conditions. Cancer-associated fibroblasts (CAFs) are major constituents of the tumour microenvironment (TME) that accompany the desmoplastic reaction responsible for anti-cancer treatment resistance. Thus, it is important to dissect the roles of CAFs in the TME to develop new therapeutic strategies for refractory cancers. Recent progress in the studies of CAF biology suggests that the functions of CAFs are complicated and that they are composed of functionally distinct populations, including cancer-promoting CAFs (pCAFs) and cancer-restraining CAFs (rCAFs). We recently identified a new cell surface marker for rCAFs in pancreatic and colon cancers, designated as Meflin (mesenchymal stromal cell- and fibroblast-expressing Linx paralogue)/Islr (immunoglobulin super family containing leucine-rich repeat). Based on the distribution of Meflin/Islr-positive cells, we also considered it a specific candidate marker for mesenchymal stroma/stem cells. Meflin/Islr-positive CAFs have been shown to suppress cancer progression by being involved in regulating collagen structures and BMP signalling in the TME. This review describes the function of Meflin/Islr in cancer fibrosis as well as in cardiac and lung fibrosis and its potential in the development of new cancer therapeutics.
Collapse
Affiliation(s)
- Masahide Takahashi
- International Center for Cell and Gene Therapy, Fujita Health University, Toyoake, Japan
| | - Hiroki Kobayashi
- Department of Pathology, Nagoya University Graduate School of Medicine, Nagoya, Japan
| | - Yasuyuki Mizutani
- Department of Gastroenterology and Hepatology, Nagoya University Graduate School of Medicine, Nagoya, Japan
| | - Akitoshi Hara
- Department of Pathology, Nagoya University Graduate School of Medicine, Nagoya, Japan
| | - Tadashi Iida
- Department of Gastroenterology and Hepatology, Nagoya University Graduate School of Medicine, Nagoya, Japan
| | - Yuki Miyai
- Department of Pathology, Nagoya University Graduate School of Medicine, Nagoya, Japan
| | - Naoya Asai
- Department of Pathology, Fujita Health University, Toyoake, Japan
| | - Atsushi Enomoto
- Department of Pathology, Nagoya University Graduate School of Medicine, Nagoya, Japan
| |
Collapse
|
|
28
|
Baxter MA, Middleton F, Cagney HP, Petty RD. Resistance to immune checkpoint inhibitors in advanced gastro-oesophageal cancers. Br J Cancer 2021; 125:1068-1079. [PMID: 34230609 PMCID: PMC8505606 DOI: 10.1038/s41416-021-01425-7] [Citation(s) in RCA: 28] [Impact Index Per Article: 9.3] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 11/09/2020] [Revised: 03/17/2021] [Accepted: 04/22/2021] [Indexed: 12/13/2022] Open
Abstract
Immune checkpoint inhibitors (ICIs) have altered the treatment paradigm across a range of tumour types, including gastro-oesophageal cancers. For patients with any cancer type who respond, ICIs can confer long-term disease control and significantly improve survival and quality of life, but for patients with gastro-oesophageal cancer, ICIs can be transformative, as durable responses in advanced disease have hitherto been rare, especially in those patients who are resistant to first-line cytotoxic therapies. Results from trials in patients with advanced-stage gastro-oesophageal cancer have raised hopes that ICIs will be successful as adjuvant and neoadjuvant treatments in early-stage disease, when the majority of patients relapse after potential curative treatments, and several trials are ongoing. Unfortunately, however, ICI-responding patients appear to constitute a minority subgroup within gastro-oesophageal cancer, and resistance to ICI therapy (whether primary or acquired) is common. Understanding the biological mechanisms of ICI resistance is a current major research challenge and involves investigation of both tumour and patient-specific factors. In this review, we discuss the mechanisms underlying ICI resistance and their potential specific applications of this knowledge towards precision medicine strategies in the management of gastro-oesophageal cancers in clinical practice.
Collapse
Affiliation(s)
- Mark A Baxter
- Division of Molecular and Clinical Medicine, Ninewells Hospital and Medical School, University of Dundee, Dundee, UK.
- Tayside Cancer Centre, Ninewells Hospital and Medical School, NHS Tayside, Dundee, UK.
| | - Fearghas Middleton
- Tayside Cancer Centre, Ninewells Hospital and Medical School, NHS Tayside, Dundee, UK
| | - Hannah P Cagney
- School of Medicine, Ninewells Hospital and Medical School, University of Dundee, Dundee, UK
| | - Russell D Petty
- Division of Molecular and Clinical Medicine, Ninewells Hospital and Medical School, University of Dundee, Dundee, UK.
- Tayside Cancer Centre, Ninewells Hospital and Medical School, NHS Tayside, Dundee, UK.
| |
Collapse
|
|
29
|
Tumor Microenvironment of Esophageal Cancer. Cancers (Basel) 2021; 13:cancers13184678. [PMID: 34572905 PMCID: PMC8472305 DOI: 10.3390/cancers13184678] [Citation(s) in RCA: 15] [Impact Index Per Article: 5.0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 08/24/2021] [Revised: 09/13/2021] [Accepted: 09/16/2021] [Indexed: 12/12/2022] Open
Abstract
Simple Summary Esophageal cancer is one of the top ten most deadly cancers. Even when diagnosed in a curable stage, patients prognosis poor. One of the parameters that is very relevant for long-term survival is response to radio(chemo)therapy prior surgery. Complete response rates are between 24 and 50 percent. This puts more than a half of every esophageal cancer patient that is diagnosed in a non-metastasized stage at high risk of recurrence. To improve response rates of treatment regimens prior curative surgery is, therefore, a major challenge in treating esophageal cancer. Not only the response of the cancer cell itself to cancer therapy is determining patients’ fate. Cells around the tumor cells called the tumor microenvironment that together with the cancer cell constitute a malignant tumor are also involved in tumor progression and therapy response. This review depicts the most important parts of the esophageal cancer microenvironment, evaluates chances and challenges of current already established therapeutic concepts that target this microenvironment. It furthermore elucidates specific pathways that are potential valuable targets in the future. Abstract Esophageal cancer is among the top ten most deadly cancers worldwide with adenocarcinomas of the esophagus showing increasing incidences over the last years. The prognosis is determined by tumor stage at diagnosis and in locally advanced stages by response to (radio-)chemotherapy followed by radical surgery. Less than a third of patients with esophageal adenocarcinomas completely respond to neoadjuvant therapies which urgently asks for further strategies to improve these rates. Aiming at the tumor microenvironment with novel targeted therapies can be one strategy to achieve this goal. This review connects experimental, translational, and clinical findings on each component of the esophageal cancer tumor microenvironment involving tumor angiogenesis, tumor-infiltrating immune cells, such as macrophages, T-cells, myeloid-derived suppressor cells, and cancer-associated fibroblasts. The review evaluates the current state of already approved concepts and depicts novel potentially targetable pathways related to esophageal cancer tumor microenvironment.
Collapse
|
|
30
|
Wang L, Han H, Wang Z, Shi L, Yang M, Qin Y. Targeting the Microenvironment in Esophageal Cancer. Front Cell Dev Biol 2021; 9:684966. [PMID: 34513829 PMCID: PMC8427432 DOI: 10.3389/fcell.2021.684966] [Citation(s) in RCA: 10] [Impact Index Per Article: 3.3] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 03/24/2021] [Accepted: 07/27/2021] [Indexed: 12/12/2022] Open
Abstract
Esophageal cancer (EC) is the eighth most common type of cancer and the sixth leading cause of cancer-related deaths worldwide. At present, the clinical treatment for EC is based mainly on radical surgery, chemotherapy, and radiotherapy. However, due to the limited efficacy of conventional treatments and the serious adverse reactions, the outcome is still unsatisfactory (the 5-year survival rate for patients is less than 25%). Thus, it is extremely important and urgent to identify new therapeutic targets. The concept of tumor microenvironment (TME) has attracted increased attention since it was proposed. Recent studies have shown that TME is an important therapeutic target for EC. Microenvironment-targeting therapies such as immunotherapy and antiangiogenic therapy have played an indispensable role in prolonging survival and improving the prognosis of patients with EC. In addition, many new drugs and therapies that have been developed to target microenvironment may become treatment options in the future. We summarize the microenvironment of EC and the latest advances in microenvironment-targeting therapies in this review.
Collapse
Affiliation(s)
- Lei Wang
- Department of Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou, China.,State Key Laboratory of Esophageal Cancer Prevention and Treatment, Zhengzhou University, Zhengzhou, China
| | - Huiqiong Han
- Department of Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou, China.,State Key Laboratory of Esophageal Cancer Prevention and Treatment, Zhengzhou University, Zhengzhou, China
| | - Zehua Wang
- Department of Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou, China.,State Key Laboratory of Esophageal Cancer Prevention and Treatment, Zhengzhou University, Zhengzhou, China
| | - Litong Shi
- Department of Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou, China.,State Key Laboratory of Esophageal Cancer Prevention and Treatment, Zhengzhou University, Zhengzhou, China
| | - Mei Yang
- Department of Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou, China.,State Key Laboratory of Esophageal Cancer Prevention and Treatment, Zhengzhou University, Zhengzhou, China
| | - Yanru Qin
- Department of Oncology, The First Affiliated Hospital of Zhengzhou University, Zhengzhou, China.,State Key Laboratory of Esophageal Cancer Prevention and Treatment, Zhengzhou University, Zhengzhou, China
| |
Collapse
|
|
31
|
Hoppe S, Jonas C, Wenzel MC, Velazquez Camacho O, Arolt C, Zhao Y, Büttner R, Quaas A, Plum PS, Hillmer AM. Genomic and Transcriptomic Characteristics of Esophageal Adenocarcinoma. Cancers (Basel) 2021; 13:cancers13174300. [PMID: 34503107 PMCID: PMC8428370 DOI: 10.3390/cancers13174300] [Citation(s) in RCA: 1] [Impact Index Per Article: 0.3] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/13/2021] [Revised: 08/20/2021] [Accepted: 08/22/2021] [Indexed: 12/28/2022] Open
Abstract
Simple Summary Cancer of the esophagus is a deadly disease. There are two main subtypes, adenocarcinoma and squamous cell carcinoma, with adenocarcinoma of the esophagus (EAC) being more common in Western countries. Barrett’s esophagus (BE) describes a change in the esophageal surface near the stomach in response to reflux of gastric acid into the esophagus. BE increases the risk of developing EAC, and the incidence of EAC has risen dramatically over recent decades. One likely reason for the poor prognosis of EAC is based on the fact that each tumor has many genes affected by mutations, and most of these genes differ across patients, hampering the efficacy of therapies that target specific cancer driver proteins. In this review, we provide an overview of the gene mutations and gene activity changes in EAC and how these features can be used to divide patients into groups that might have different clinical characteristics. Abstract Esophageal adenocarcinoma (EAC) is a deadly disease with limited options for targeted therapy. With the help of next-generation sequencing studies over the last decade, we gained an understanding of the genomic architecture of EAC. The tumor suppressor gene TP53 is mutated in 70 to 80% of tumors followed by genomic alterations in CDKN2A, KRAS, ERBB2, ARID1A, SMAD4 and a long tail of less frequently mutated genes. EAC is characterized by a high burden of point mutations and genomic rearrangements, resulting in amplifications and deletions of genomic regions. The genomic complexity is likely hampering the efficacy of targeted therapies. Barrett’s esophagus (BE), a metaplastic response of the esophagus to gastro-esophageal reflux disease, is the main risk factor for the development of EAC. Almost all EACs are derived from BE. The sequence from BE to EAC provides an opportunity to study the genomic evolution towards EAC. While the overlap of point mutations between BE and EAC within the same patient is, at times, surprisingly low, there is a correlation between the complexity of the genomic copy number profile and the development of EAC. Transcriptomic analyses separated EAC into a basal and a classical subtype, with the basal subtype showing a higher level of resistance to chemotherapy. In this review, we provide an overview of the current knowledge of the genomic and transcriptomic characteristics of EAC and their relevance for the development of the disease and patient care.
Collapse
Affiliation(s)
- Sascha Hoppe
- Institute of Pathology, Faculty of Medicine and University Hospital Cologne, University of Cologne, 50937 Cologne, Germany; (S.H.); (C.J.); (M.C.W.); (O.V.C.); (C.A.); (R.B.); (A.Q.); (P.S.P.)
| | - Christoph Jonas
- Institute of Pathology, Faculty of Medicine and University Hospital Cologne, University of Cologne, 50937 Cologne, Germany; (S.H.); (C.J.); (M.C.W.); (O.V.C.); (C.A.); (R.B.); (A.Q.); (P.S.P.)
| | - Marten Christian Wenzel
- Institute of Pathology, Faculty of Medicine and University Hospital Cologne, University of Cologne, 50937 Cologne, Germany; (S.H.); (C.J.); (M.C.W.); (O.V.C.); (C.A.); (R.B.); (A.Q.); (P.S.P.)
| | - Oscar Velazquez Camacho
- Institute of Pathology, Faculty of Medicine and University Hospital Cologne, University of Cologne, 50937 Cologne, Germany; (S.H.); (C.J.); (M.C.W.); (O.V.C.); (C.A.); (R.B.); (A.Q.); (P.S.P.)
| | - Christoph Arolt
- Institute of Pathology, Faculty of Medicine and University Hospital Cologne, University of Cologne, 50937 Cologne, Germany; (S.H.); (C.J.); (M.C.W.); (O.V.C.); (C.A.); (R.B.); (A.Q.); (P.S.P.)
| | - Yue Zhao
- Department of General, Visceral, Cancer and Transplantation Surgery, Faculty of Medicine and University Hospital Cologne, University of Cologne, 50937 Cologne, Germany;
| | - Reinhard Büttner
- Institute of Pathology, Faculty of Medicine and University Hospital Cologne, University of Cologne, 50937 Cologne, Germany; (S.H.); (C.J.); (M.C.W.); (O.V.C.); (C.A.); (R.B.); (A.Q.); (P.S.P.)
| | - Alexander Quaas
- Institute of Pathology, Faculty of Medicine and University Hospital Cologne, University of Cologne, 50937 Cologne, Germany; (S.H.); (C.J.); (M.C.W.); (O.V.C.); (C.A.); (R.B.); (A.Q.); (P.S.P.)
| | - Patrick Sven Plum
- Institute of Pathology, Faculty of Medicine and University Hospital Cologne, University of Cologne, 50937 Cologne, Germany; (S.H.); (C.J.); (M.C.W.); (O.V.C.); (C.A.); (R.B.); (A.Q.); (P.S.P.)
- Department of General, Visceral, Cancer and Transplantation Surgery, Faculty of Medicine and University Hospital Cologne, University of Cologne, 50937 Cologne, Germany;
| | - Axel Maximilian Hillmer
- Institute of Pathology, Faculty of Medicine and University Hospital Cologne, University of Cologne, 50937 Cologne, Germany; (S.H.); (C.J.); (M.C.W.); (O.V.C.); (C.A.); (R.B.); (A.Q.); (P.S.P.)
- Center for Molecular Medicine Cologne, University of Cologne, 50931 Cologne, Germany
- Correspondence:
| |
Collapse
|
|
32
|
Pickering OJ, Breininger SP, Underwood TJ, Walters ZS. Histone Modifying Enzymes as Targets for Therapeutic Intervention in Oesophageal Adenocarcinoma. Cancers (Basel) 2021; 13:4084. [PMID: 34439236 PMCID: PMC8392153 DOI: 10.3390/cancers13164084] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Key Words] [Grants] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 06/28/2021] [Revised: 08/03/2021] [Accepted: 08/10/2021] [Indexed: 12/24/2022] Open
Abstract
Oesophageal adenocarcinoma (OAC) has a dismal prognosis, where curable disease occurs in less than 40% of patients, and many of those with incurable disease survive for less than a year from diagnosis. Despite the widespread use of systematic chemotherapy in OAC treatment, many patients receive no benefit. New treatments are urgently needed for OAC patients. There is an emerging interest in epigenetic regulators in cancer pathogenesis, which are now translating into novel cancer therapeutic strategies. Histone-modifying enzymes (HMEs) are key epigenetic regulators responsible for dynamic covalent histone modifications that play roles in both normal and dysregulated cellular processes including tumorigenesis. Several HME inhibitors are in clinical use for haematological malignancies and sarcomas, with numerous on-going clinical trials for their use in solid tumours. This review discusses the current literature surrounding HMEs in OAC pathogenesis and their potential use in targeted therapies for this disease.
Collapse
Affiliation(s)
| | | | | | - Zoë S. Walters
- School of Cancer Sciences, Faculty of Medicine, University of Southampton, Southampton SO17 1BJ, UK; (O.J.P.); (S.P.B.); (T.J.U.)
| |
Collapse
|
|
33
|
Davern M, Donlon NE, Power R, Hayes C, King R, Dunne MR, Reynolds JV. The tumour immune microenvironment in oesophageal cancer. Br J Cancer 2021; 125:479-494. [PMID: 33903730 PMCID: PMC8368180 DOI: 10.1038/s41416-021-01331-y] [Citation(s) in RCA: 18] [Impact Index Per Article: 6.0] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 07/26/2020] [Revised: 01/16/2021] [Accepted: 02/17/2021] [Indexed: 02/02/2023] Open
Abstract
Oesophageal cancer (OC) is an inflammation-associated malignancy linked to gastro-oesophageal reflux disease, obesity and tobacco use. Knowledge of the microenvironment of oesophageal tumours is relevant to our understanding of the development of OC and its biology, and has major implications for understanding the response to standard therapies and immunotherapies, as well as for uncovering novel targets. In this context, we discuss what is known about the TME in OC from tumour initiation to development and progression, and how this is relevant to therapy sensitivity and resistance in the two major types of OC. We provide an immunological characterisation of the OC TME and discuss its prognostic implications with specific comparison with the Immunoscore and immune-hot, -cold, altered-immunosuppressed and -altered-excluded models. Targeted therapeutics for the TME under pre-clinical and clinical investigation in OCs are also summarised. A deeper understanding of the TME will enable the development of combination approaches to concurrently target the tumour cells and TME delivering precision medicine to OC patients.
Collapse
Affiliation(s)
- Maria Davern
- Department of Surgery, School of Medicine, Trinity College Dublin, Dublin, Ireland
- Trinity St James's Cancer Institute, St James's Hospital, Dublin, Ireland
| | - Noel E Donlon
- Department of Surgery, School of Medicine, Trinity College Dublin, Dublin, Ireland
- Trinity St James's Cancer Institute, St James's Hospital, Dublin, Ireland
| | - Robert Power
- Department of Surgery, School of Medicine, Trinity College Dublin, Dublin, Ireland
- Trinity St James's Cancer Institute, St James's Hospital, Dublin, Ireland
| | - Conall Hayes
- Department of Surgery, School of Medicine, Trinity College Dublin, Dublin, Ireland
- Trinity St James's Cancer Institute, St James's Hospital, Dublin, Ireland
| | - Ross King
- Department of Surgery, School of Medicine, Trinity College Dublin, Dublin, Ireland
- Trinity St James's Cancer Institute, St James's Hospital, Dublin, Ireland
| | - Margaret R Dunne
- Department of Surgery, School of Medicine, Trinity College Dublin, Dublin, Ireland
- Trinity St James's Cancer Institute, St James's Hospital, Dublin, Ireland
| | - John V Reynolds
- Department of Surgery, School of Medicine, Trinity College Dublin, Dublin, Ireland.
- Trinity St James's Cancer Institute, St James's Hospital, Dublin, Ireland.
| |
Collapse
|
|
34
|
McShane R, Arya S, Stewart AJ, Caie P, Bates M. Prognostic features of the tumour microenvironment in oesophageal adenocarcinoma. Biochim Biophys Acta Rev Cancer 2021; 1876:188598. [PMID: 34332022 DOI: 10.1016/j.bbcan.2021.188598] [Citation(s) in RCA: 10] [Impact Index Per Article: 3.3] [Reference Citation Analysis] [Abstract] [Key Words] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/08/2021] [Revised: 07/26/2021] [Accepted: 07/26/2021] [Indexed: 12/12/2022]
Abstract
Oesophageal adenocarcinoma (OAC) is a disease with an incredibly poor survival rate and a complex makeup. The growth and spread of OAC tumours are profoundly influenced by their surrounding microenvironment and the properties of the tumour itself. Constant crosstalk between the tumour and its microenvironment is key to the survival of the tumour and ultimately the death of the patient. The tumour microenvironment (TME) is composed of a complex milieu of cell types including cancer associated fibroblasts (CAFs) which make up the tumour stroma, endothelial cells which line blood and lymphatic vessels and infiltrating immune cell populations. These various cell types and the tumour constantly communicate through environmental cues including fluctuations in pH, hypoxia and the release of mitogens such as cytokines, chemokines and growth factors, many of which help promote malignant progression. Eventually clusters of tumour cells such as tumour buds break away and spread through the lymphatic system to nearby lymph nodes or enter the circulation forming secondary metastasis. Collectively, these factors need to be considered when assessing and treating patients clinically. This review aims to summarise the ways in which these various factors are currently assessed and how they relate to patient treatment and outcome at an individual level.
Collapse
Affiliation(s)
| | - Swati Arya
- School of Medicine, University of St Andrews, Fife, UK
| | | | - Peter Caie
- School of Medicine, University of St Andrews, Fife, UK
| | - Mark Bates
- Department of Surgery, Trinity Translational Medicine Institute, St. James's Hospital, Dublin 8, Ireland; Trinity St James's Cancer Institute, St James's Hospital, Dublin 8, Ireland.
| |
Collapse
|
|
35
|
Ansardamavandi A, Tafazzoli-Shadpour M. The functional cross talk between cancer cells and cancer associated fibroblasts from a cancer mechanics perspective. BIOCHIMICA ET BIOPHYSICA ACTA-MOLECULAR CELL RESEARCH 2021; 1868:119103. [PMID: 34293346 DOI: 10.1016/j.bbamcr.2021.119103] [Citation(s) in RCA: 15] [Impact Index Per Article: 5.0] [Reference Citation Analysis] [Abstract] [Key Words] [Subscribe] [Scholar Register] [Received: 06/04/2021] [Revised: 07/13/2021] [Accepted: 07/18/2021] [Indexed: 12/12/2022]
Abstract
The function of biological tissues in health and disease is regulated at cellular level and is highly influenced by the physical microenvironment, through the interaction of forces between cells and ECM, which are perceived through mechanosensing pathways. In cancer, both chemical and physical signaling cascades and their interactions are involved during cell-cell and cell-ECM communications to meet requirements of tumor growth. Among stroma cells, cancer associated fibroblasts (CAFs) play key role in tumor growth and pave the way for cancer cells to initiate metastasis and invasion to other tissues, and without recruitment of CAFs, the process of cancer invasion is dysfunctional. This is through an intense chemical and physical cross talks with tumor cells, and interactive remodeling of ECM. During such interaction CAFs apply traction forces and depending on the mechanical properties, deform ECM and in return receive physical signals from the micromechanical environment. Such interaction leads to ECM remodeling by manipulating ECM structure and its mechanical properties. The results are in form of deposition of extra fibers, stiffening, rearrangement and reorganization of fibrous structure, and degradation which are due to a complex secretion and expression of different markers triggered by mechanosensing of tumor cells, specially CAFs. Such events define cancer progress and invasion of cancer cells. A systemic knowledge of chemical and physical factors provides a holistic view of how cancer process and enhances the current treatment methods to provide more diversity among targets that involves tumor cells and ECM structure.
Collapse
Affiliation(s)
- Arian Ansardamavandi
- Faculty of Biomedical Engineering, Amirkabir University of Technology, Tehran, Iran
| | | |
Collapse
|
|
36
|
TGF-β Signaling: From Tissue Fibrosis to Tumor Microenvironment. Int J Mol Sci 2021; 22:ijms22147575. [PMID: 34299192 PMCID: PMC8303588 DOI: 10.3390/ijms22147575] [Citation(s) in RCA: 85] [Impact Index Per Article: 28.3] [Reference Citation Analysis] [Abstract] [Key Words] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 05/24/2021] [Revised: 07/09/2021] [Accepted: 07/09/2021] [Indexed: 02/06/2023] Open
Abstract
Transforming growth factor-β (TGF-β) signaling triggers diverse biological actions in inflammatory diseases. In tissue fibrosis, it acts as a key pathogenic regulator for promoting immunoregulation via controlling the activation, proliferation, and apoptosis of immunocytes. In cancer, it plays a critical role in tumor microenvironment (TME) for accelerating invasion, metastasis, angiogenesis, and immunosuppression. Increasing evidence suggest a pleiotropic nature of TGF-β signaling as a critical pathway for generating fibrotic TME, which contains numerous cancer-associated fibroblasts (CAFs), extracellular matrix proteins, and remodeling enzymes. Its pathogenic roles and working mechanisms in tumorigenesis are still largely unclear. Importantly, recent studies successfully demonstrated the clinical implications of fibrotic TME in cancer. This review systematically summarized the latest updates and discoveries of TGF-β signaling in the fibrotic TME.
Collapse
|
|
37
|
Hanley CJ, Thomas GJ. Targeting cancer associated fibroblasts to enhance immunotherapy: emerging strategies and future perspectives. Oncotarget 2021; 12:1427-1433. [PMID: 34262652 PMCID: PMC8274722 DOI: 10.18632/oncotarget.27936] [Citation(s) in RCA: 22] [Impact Index Per Article: 7.3] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Journal Information] [Subscribe] [Scholar Register] [Received: 03/23/2021] [Accepted: 03/24/2021] [Indexed: 12/26/2022] Open
Abstract
Cancer associated fibroblasts are a prominent component of the tumour microenvironment in most solid cancers. This heterogeneous population of cells are known to play an important role in tumour progression and recent studies have demonstrated that CAFs may confer resistance to checkpoint immunotherapy, suggesting that targeting these cells could improve response rates. However, effective clinical strategies for CAF targeting have yet to be identified. In this editorial, we highlight current limitations in our understanding of CAF heterogeneity, and discuss the potential and possible approaches for CAF-directed therapy.
Collapse
Affiliation(s)
| | - Gareth J Thomas
- School of Cancer Sciences, University of Southampton, Southampton, UK.,Cancer Research UK and NIHR Southampton Experimental Cancer Medicine Centre, Southampton, UK
| |
Collapse
|
|
38
|
Wu F, Yang J, Liu J, Wang Y, Mu J, Zeng Q, Deng S, Zhou H. Signaling pathways in cancer-associated fibroblasts and targeted therapy for cancer. Signal Transduct Target Ther 2021; 6:218. [PMID: 34108441 PMCID: PMC8190181 DOI: 10.1038/s41392-021-00641-0] [Citation(s) in RCA: 251] [Impact Index Per Article: 83.7] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/18/2021] [Revised: 04/20/2021] [Accepted: 05/06/2021] [Indexed: 02/05/2023] Open
Abstract
To flourish, cancers greatly depend on their surrounding tumor microenvironment (TME), and cancer-associated fibroblasts (CAFs) in TME are critical for cancer occurrence and progression because of their versatile roles in extracellular matrix remodeling, maintenance of stemness, blood vessel formation, modulation of tumor metabolism, immune response, and promotion of cancer cell proliferation, migration, invasion, and therapeutic resistance. CAFs are highly heterogeneous stromal cells and their crosstalk with cancer cells is mediated by a complex and intricate signaling network consisting of transforming growth factor-beta, phosphoinositide 3-kinase/AKT/mammalian target of rapamycin, mitogen-activated protein kinase, Wnt, Janus kinase/signal transducers and activators of transcription, epidermal growth factor receptor, Hippo, and nuclear factor kappa-light-chain-enhancer of activated B cells, etc., signaling pathways. These signals in CAFs exhibit their own special characteristics during the cancer progression and have the potential to be targeted for anticancer therapy. Therefore, a comprehensive understanding of these signaling cascades in interactions between cancer cells and CAFs is necessary to fully realize the pivotal roles of CAFs in cancers. Herein, in this review, we will summarize the enormous amounts of findings on the signals mediating crosstalk of CAFs with cancer cells and its related targets or trials. Further, we hypothesize three potential targeting strategies, including, namely, epithelial-mesenchymal common targets, sequential target perturbation, and crosstalk-directed signaling targets, paving the way for CAF-directed or host cell-directed antitumor therapy.
Collapse
Affiliation(s)
- Fanglong Wu
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, West China Hospital of Stomatology, Sichuan University, Chengdu, Sichuan, People's Republic of China
| | - Jin Yang
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, West China Hospital of Stomatology, Sichuan University, Chengdu, Sichuan, People's Republic of China
| | - Junjiang Liu
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, West China Hospital of Stomatology, Sichuan University, Chengdu, Sichuan, People's Republic of China
| | - Ye Wang
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, West China Hospital of Stomatology, Sichuan University, Chengdu, Sichuan, People's Republic of China
| | - Jingtian Mu
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, West China Hospital of Stomatology, Sichuan University, Chengdu, Sichuan, People's Republic of China
| | - Qingxiang Zeng
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, West China Hospital of Stomatology, Sichuan University, Chengdu, Sichuan, People's Republic of China
| | - Shuzhi Deng
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, West China Hospital of Stomatology, Sichuan University, Chengdu, Sichuan, People's Republic of China
| | - Hongmei Zhou
- State Key Laboratory of Oral Diseases, National Center of Stomatology, National Clinical Research Center for Oral Diseases, West China Hospital of Stomatology, Sichuan University, Chengdu, Sichuan, People's Republic of China.
| |
Collapse
|
|
39
|
King R, Hayes C, Donohoe CL, Dunne MR, Davern M, Donlon NE. Hypoxia and its impact on the tumour microenvironment of gastroesophageal cancers. World J Gastrointest Oncol 2021; 13:312-331. [PMID: 34040696 PMCID: PMC8131902 DOI: 10.4251/wjgo.v13.i5.312] [Citation(s) in RCA: 7] [Impact Index Per Article: 2.3] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Journal Information] [Submit a Manuscript] [Subscribe] [Scholar Register] [Received: 12/27/2020] [Revised: 02/24/2021] [Accepted: 04/14/2021] [Indexed: 02/06/2023] Open
Abstract
The malfeasant role of the hypoxic tumour microenvironment (TME) in cancer progression was recognized decades ago but the exact mechanisms that augment the hallmarks of cancer and promote treatment resistance continue to be elucidated. Gastroesophageal cancers (GOCs) represent a major burden of worldwide disease, responsible for the deaths of over 1 million people annually. Disentangling the impact of hypoxia in GOCs enables a better overall understanding of the disease pathogenesis while shining a light on novel therapeutic strategies and facilitating precision treatment approaches with the ultimate goal of improving outcomes for patients with these diseases. This review discusses the underlying principles and processes of the hypoxic response and the effect of hypoxia in promoting the hallmarks of cancer in the context of GOCs. We focus on its bidirectional influence on inflammation and how it drives angiogenesis, innate and adaptive immune evasion, metastasis, and the reprogramming of cellular bioenergetics. The contribution of the hypoxic GOC TME to treatment resistance is examined and a brief overview of the pharmacodynamics of hypoxia-targeted therapeutics is given. The principal methods that are used in measuring hypoxia and how they may enhance prognostication or provide rationale for individually tailored management in the case of tumours with significant hypoxic regions are also discussed.
Collapse
Affiliation(s)
- Ross King
- Department of Surgery, St. James’s Hospital Campus, Trinity Translational Medicine Institute, Dublin D8, Ireland
| | - Conall Hayes
- Department of Surgery, St. James’s Hospital Campus, Trinity Translational Medicine Institute, Dublin D8, Ireland
| | - Claire L Donohoe
- Department of Surgery, St. James’s Hospital Campus, Trinity Translational Medicine Institute, Dublin D8, Ireland
| | - Margaret R Dunne
- Department of Surgery, St. James’s Hospital Campus, Trinity Translational Medicine Institute, Dublin D8, Ireland
| | - Maria Davern
- Department of Surgery, St. James’s Hospital Campus, Trinity Translational Medicine Institute, Dublin D8, Ireland
| | - Noel E Donlon
- Department of Surgery, St. James’s Hospital Campus, Trinity Translational Medicine Institute, Dublin D8, Ireland
| |
Collapse
|
|
40
|
Baker AT, Abuwarwar MH, Poly L, Wilkins S, Fletcher AL. Cancer-Associated Fibroblasts and T Cells: From Mechanisms to Outcomes. THE JOURNAL OF IMMUNOLOGY 2021; 206:310-320. [PMID: 33397745 DOI: 10.4049/jimmunol.2001203] [Citation(s) in RCA: 30] [Impact Index Per Article: 10.0] [Reference Citation Analysis] [Abstract] [Track Full Text] [Subscribe] [Scholar Register] [Received: 10/23/2020] [Accepted: 11/06/2020] [Indexed: 12/20/2022]
Abstract
Over the past decade, T cell immunotherapy has changed the face of cancer treatment, providing robust treatment options for several previously intractable cancers. Unfortunately, many epithelial tumors with high mortality rates respond poorly to immunotherapy, and an understanding of the key impediments is urgently required. Cancer-associated fibroblasts (CAFs) comprise the most frequent nonneoplastic cellular component in most solid tumors. Far from an inert scaffold, CAFs significantly influence tumor neogenesis, persistence, and metastasis and are emerging as a key player in immunotherapy resistance. In this review, we discuss the physical and chemical barriers that CAFs place between effector T cells and their tumor cell targets, and the therapies poised to target them.
Collapse
Affiliation(s)
- Alfie T Baker
- Department of Biochemistry and Molecular Biology, Monash Biomedicine Discovery Institute, Monash University, Clayton 3800, Victoria, Australia
| | - Mohammed H Abuwarwar
- Department of Biochemistry and Molecular Biology, Monash Biomedicine Discovery Institute, Monash University, Clayton 3800, Victoria, Australia
| | - Lylarath Poly
- Department of Biochemistry and Molecular Biology, Monash Biomedicine Discovery Institute, Monash University, Clayton 3800, Victoria, Australia
| | - Simon Wilkins
- Cabrini Monash University Department of Surgery, Cabrini Hospital, Malvern 3144, Victoria, Australia.,Department of Epidemiology and Preventive Medicine, School of Public Health and Preventive Medicine, Monash University, Melbourne 3004, Victoria, Australia; and
| | - Anne L Fletcher
- Department of Biochemistry and Molecular Biology, Monash Biomedicine Discovery Institute, Monash University, Clayton 3800, Victoria, Australia; .,Institute of Immunology and Immunotherapy, University of Birmingham, Edgbaston B15 2TT, United Kingdom
| |
Collapse
|
|
41
|
Lonie JM, Barbour AP, Dolcetti R. Understanding the immuno-biology of oesophageal adenocarcinoma: Towards improved therapeutic approaches. Cancer Treat Rev 2021; 98:102219. [PMID: 33993033 DOI: 10.1016/j.ctrv.2021.102219] [Citation(s) in RCA: 4] [Impact Index Per Article: 1.3] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 03/28/2021] [Revised: 04/30/2021] [Accepted: 05/05/2021] [Indexed: 12/12/2022]
Abstract
With an incidence that is constantly rising, oesophageal adenocarcinoma (OAC) is becoming an increasing health burden worldwide. Although significant advances in treatment regimens have improved patient outcomes, survival rates for this deadly cancer remain unsatisfactory. This highlights the need to improve current therapeutic approaches and develop novel therapeutic strategies for treating OAC patients. The advent of immunotherapy has revolutionised treatment across a range of malignancies, however outcomes in OAC show modest results. The inherent resistance of OAC to treatment reflects the complex genomic landscape of this cancer, which displays a lack of ubiquitous driver mutations and large-scale genomic alterations along with high tumour and immune heterogeneity. Research into the immune landscape of OAC is limited, and elucidation of the mechanisms surrounding the immune responses to this complex cancer will result in improved therapeutic approaches. This review explores what is known about the immuno-biology of OAC and explores promising therapeutic avenues that may improve responses to immunotherapeutic regimens.
Collapse
Affiliation(s)
- James M Lonie
- The University of Queensland Diamantina Institute, Translational Research Institute, Brisbane, Queensland, Australia.
| | - Andrew P Barbour
- The University of Queensland Diamantina Institute, Translational Research Institute, Brisbane, Queensland, Australia; Princess Alexandra Hospital, Brisbane, Queensland, Australia
| | - Riccardo Dolcetti
- The University of Queensland Diamantina Institute, Translational Research Institute, Brisbane, Queensland, Australia; Sir Peter MacCallum Cancer Centre, The University of Melbourne, Melbourne, Victoria, Australia
| |
Collapse
|
|
42
|
Ikeda-Iwabu Y, Taniyama Y, Katsuragi N, Sanada F, Koibuchi N, Shibata K, Shimazu K, Rakugi H, Morishita R. Periostin Short Fragment with Exon 17 via Aberrant Alternative Splicing Is Required for Breast Cancer Growth and Metastasis. Cells 2021; 10:892. [PMID: 33919736 PMCID: PMC8070743 DOI: 10.3390/cells10040892] [Citation(s) in RCA: 3] [Impact Index Per Article: 1.0] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Grants] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/31/2021] [Revised: 04/09/2021] [Accepted: 04/12/2021] [Indexed: 12/26/2022] Open
Abstract
BACKGROUND Periostin (POSTN) is a 93 kDa matrix protein that helps to regulate collagen gene expression in the extracellular matrix. POSTN overexpression is a prognostic factor in malignant cancers; however, some researchers have observed it in the stroma, whereas others have reported it on tumors. OBJECTIVE This study aimed to investigate the function of POSTN on tumors. METHODS AND RESULTS We found that POSTN in cancer cells can be detected by using an antibody against the POSTN C-terminal region exon 17 (Ex17 antibody), but not with an antibody against the POSTN N-terminal region exon 12 (Ex12 antibody) in patients with breast cancer. In a fraction secreted from fibroblasts, LC-MS/MS analysis revealed a short fragment of POSTN of approximately 40 kDa with exon 17. In addition, molecular interaction analysis showed that POSTN with exon 17, but not POSTN without exon 17, bound specifically to wnt3a, and the Ex17 antibody inhibited the binding. CONCLUSION A short fragment of POSTN with exon 17, which originates in the fibroblasts, is transported to cancer cells, whereas POSTN fragments without exon 17 are retained in the stroma. The Ex17 antibody inhibits the binding between POSTN exon 17 and wnt3a.
Collapse
Affiliation(s)
- Yuka Ikeda-Iwabu
- Department of Clinical Gene Therapy, Osaka University Graduate School of Medicine, Suita, Osaka 565-0871, Japan; (Y.I.-I.); (N.K.); (F.S.); (N.K.); (K.S.)
| | - Yoshiaki Taniyama
- Department of Clinical Gene Therapy, Osaka University Graduate School of Medicine, Suita, Osaka 565-0871, Japan; (Y.I.-I.); (N.K.); (F.S.); (N.K.); (K.S.)
- Department of Geriatric and General Medicine, Osaka University Graduate School of Medicine, Suita, Osaka 565-0871, Japan;
| | - Naruto Katsuragi
- Department of Clinical Gene Therapy, Osaka University Graduate School of Medicine, Suita, Osaka 565-0871, Japan; (Y.I.-I.); (N.K.); (F.S.); (N.K.); (K.S.)
| | - Fumihiro Sanada
- Department of Clinical Gene Therapy, Osaka University Graduate School of Medicine, Suita, Osaka 565-0871, Japan; (Y.I.-I.); (N.K.); (F.S.); (N.K.); (K.S.)
| | - Nobutaka Koibuchi
- Department of Clinical Gene Therapy, Osaka University Graduate School of Medicine, Suita, Osaka 565-0871, Japan; (Y.I.-I.); (N.K.); (F.S.); (N.K.); (K.S.)
| | - Kana Shibata
- Department of Clinical Gene Therapy, Osaka University Graduate School of Medicine, Suita, Osaka 565-0871, Japan; (Y.I.-I.); (N.K.); (F.S.); (N.K.); (K.S.)
| | - Kenzo Shimazu
- Department of Breast and Endocrine Surgery, Osaka University Graduate School of Medicine, Suita, Osaka 565-0871, Japan;
| | - Hiromi Rakugi
- Department of Geriatric and General Medicine, Osaka University Graduate School of Medicine, Suita, Osaka 565-0871, Japan;
| | - Ryuichi Morishita
- Department of Clinical Gene Therapy, Osaka University Graduate School of Medicine, Suita, Osaka 565-0871, Japan; (Y.I.-I.); (N.K.); (F.S.); (N.K.); (K.S.)
| |
Collapse
|
|
43
|
Yamauchi N, Kanke Y, Saito K, Okayama H, Yamada S, Nakajima S, Endo E, Kase K, Yamada L, Nakano H, Matsumoto T, Hanayama H, Watanabe Y, Hayase S, Saito M, Saze Z, Mimura K, Momma T, Oki S, Hashimoto Y, Kono K. Stromal expression of cancer-associated fibroblast-related molecules, versican and lumican, is strongly associated with worse relapse-free and overall survival times in patients with esophageal squamous cell carcinoma. Oncol Lett 2021; 21:445. [PMID: 33868483 PMCID: PMC8045151 DOI: 10.3892/ol.2021.12706] [Citation(s) in RCA: 13] [Impact Index Per Article: 4.3] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 09/19/2020] [Accepted: 02/26/2021] [Indexed: 12/24/2022] Open
Abstract
Cancer-associated fibroblasts (CAFs) in the tumor microenvironment play an essential role in the tumor progression of esophageal squamous cell carcinoma (ESCC). The present study aimed to investigate the expression of CAF-related molecules, versican, periostin and lumican, in cancer stroma, to provide prognostic stratification for patients with ESCC after surgery. A total of 106 patients with ESCC who underwent curative esophagectomy without preoperative chemotherapy or radiotherapy were enrolled. The expression of CAF-related stromal proteins, including versican, periostin and lumican, was examined using immunohistochemistry, and the prognostic value was assessed by Kaplan-Meier survival analysis, and univariate and multivariate Cox regression models. The expression of versican, periostin and lumican was found specifically in the stromal component of ESCC. Kaplan-Meier analysis demonstrated that, compared with a low expression level, a high expression level of versican, periostin or lumican in the cancer stroma was significantly associated with worse relapse-free survival (RFS) and overall survival times in patients with ESCC. The prognostic values of stromal versican and lumican remained significant in a stratified analysis of stage I patients. Moreover, univariate and multivariate analysis revealed that high stromal versican or lumican expression was an independent prognostic factor for RFS in the patients. The present study demonstrated that CAF-related molecules, including versican, periostin and lumican, were expressed in the stroma of ESCC, and that stromal expression of versican and lumican in particular may have clinical utility as a prognostic biomarker for poor RFS in postoperative patients with ESCC.
Collapse
Affiliation(s)
- Naoto Yamauchi
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Yasuyuki Kanke
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Katsuharu Saito
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Hirokazu Okayama
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Shoki Yamada
- Department of Diagnostic Pathology, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Shotaro Nakajima
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Eisei Endo
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Koji Kase
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Leo Yamada
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Hiroshi Nakano
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Takuro Matsumoto
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Hiroyuki Hanayama
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Yohei Watanabe
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Suguru Hayase
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Motonobu Saito
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Zenichiro Saze
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Kosaku Mimura
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Tomoyuki Momma
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Shinji Oki
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Yuko Hashimoto
- Department of Diagnostic Pathology, Fukushima Medical University, Fukushima 960-1295, Japan
| | - Koji Kono
- Department of Gastrointestinal Tract Surgery, Fukushima Medical University, Fukushima 960-1295, Japan
| |
Collapse
|
|
44
|
An integrated approach for identification of a panel of candidate genes arbitrated for invasion and metastasis in oral squamous cell carcinoma. Sci Rep 2021; 11:6208. [PMID: 33739025 PMCID: PMC7973753 DOI: 10.1038/s41598-021-85729-x] [Citation(s) in RCA: 0] [Impact Index Per Article: 0] [Reference Citation Analysis] [Abstract] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 04/22/2020] [Accepted: 03/01/2021] [Indexed: 12/24/2022] Open
Abstract
Oral squamous cell carcinoma (OSCC) is known for its aggressiveness associated with poor prognosis. The molecular mechanisms underlying the invasion and metastasis are still poorly understood. An improved understanding of these mechanisms shall precede the development of new diagnostic tools and targeted therapies. We report an integrated approach using bioinformatics to predict candidate genes, coupled with proteomics and immunohistochemistry for validating their presence and involvement in OSCC pathways heralding invasion and metastasis. Four genes POSTN, TNC, CAV1 and FSCN1 were identified. A protein–protein interaction network analysis teamed with pathway analysis led us to propose the role of the identified genes in invasion and metastasis in OSCC. Further analyses of archived FFPE blocks of various grades of oral cancer was carried out using TMT-based mass spectrometry and immunohistochemistry. Results of this study expressed a strong communiqué and interrelationship between these candidate genes. This study emphasizes the significance of a molecular biomarker panel as a diagnostic tool and its correlation with the invasion and metastatic pathway of OSCC. An insight into the probable association of CAF's and these biomarkers in the evolution and malignant transformation of OSCC further magnifies the molecular-biological spectrum of OSCC tumour microenvironment.
Collapse
|
|
45
|
Tumor-secreted exosomal Wnt2B activates fibroblasts to promote cervical cancer progression. Oncogenesis 2021; 10:30. [PMID: 33731705 PMCID: PMC7969781 DOI: 10.1038/s41389-021-00319-w] [Citation(s) in RCA: 23] [Impact Index Per Article: 7.7] [Reference Citation Analysis] [Abstract] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 02/07/2020] [Revised: 02/11/2021] [Accepted: 02/26/2021] [Indexed: 01/28/2023] Open
Abstract
The activation of stromal fibroblasts into cancer-associated fibroblasts (CAFs) has been suggested to promote primary tumor growth and progression; however, the mechanisms underlying the crosstalk between tumors and fibroblasts that drives stromal heterogeneity remain unknown. Here, we show that high Wnt2B levels were positively correlated with the number of CAFs in cervical cancer (CC). More importantly, Wnt2B was characteristically enriched in CC cell-secreted exosomes and transferred into fibroblasts to promote fibroblast activation via Wnt/β-catenin signaling, and inhibiting exosomal release or the Wnt/β-catenin signaling pathway diminished the activation induced by exosomal Wnt2B. Moreover, circulating exosomal Wnt2B also promoted CAF conversion in vitro and its expression was significantly higher in CC patients. In conclusion, our findings indicate that CC cell-derived Wnt2B can induce the activation of fibroblasts into CAFs, mainly via exosome-dependent secretion, thus providing directions for the development of diagnostic and therapeutic targets for CC progression.
Collapse
|
|
46
|
Sunami Y, Böker V, Kleeff J. Targeting and Reprograming Cancer-Associated Fibroblasts and the Tumor Microenvironment in Pancreatic Cancer. Cancers (Basel) 2021; 13:697. [PMID: 33572223 PMCID: PMC7915918 DOI: 10.3390/cancers13040697] [Citation(s) in RCA: 20] [Impact Index Per Article: 6.7] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 01/11/2021] [Revised: 02/04/2021] [Accepted: 02/05/2021] [Indexed: 02/07/2023] Open
Abstract
Pancreatic cancer is the fourth leading cause of cancer deaths in the United States both in female and male, and is projected to become the second deadliest cancer by 2030. The overall five-year survival rate remains at around 10%. Pancreatic cancer exhibits a remarkable resistance to established therapeutic options such as chemotherapy and radiotherapy, due to dense stromal tumor microenvironment. Cancer-associated fibroblasts are the major stromal cell type and source of extracellular matrix proteins shaping a physical and metabolic barrier thereby reducing therapeutic efficacy. Targeting cancer-associated fibroblasts has been considered a promising therapeutic strategy. However, depleting cancer-associated fibroblasts may also have tumor-promoting effects due to their functional heterogeneity. Several subtypes of cancer-associated fibroblasts have been suggested to exhibit tumor-restraining function. This review article summarizes recent preclinical and clinical investigations addressing pancreatic cancer therapy through targeting specific subtypes of cancer-associated fibroblasts, deprogramming activated fibroblasts, administration of mesenchymal stem cells, as well as reprogramming tumor-promoting cancer-associated fibroblasts to tumor-restraining cancer-associated fibroblasts. Further, inter-cellular mediators between cancer-associated fibroblasts and the surrounding tissue microenvironment are discussed. It is important to increase our understanding of cancer-associated fibroblast heterogeneity and the tumor microenvironment for more specific and personalized therapies for pancreatic cancer patients in the future.
Collapse
Affiliation(s)
- Yoshiaki Sunami
- Department of Visceral, Vascular and Endocrine Surgery, Martin-Luther-University Halle-Wittenberg, University Medical Center Halle, 06120 Halle, Germany; (V.B.); (J.K.)
| | | | | |
Collapse
|
|
47
|
Jin Y, Meng Q, Zhang B, Xie C, Chen X, Tian B, Wang J, Shih TC, Zhang Y, Cao J, Yang Y, Chen S, Guan X, Chen X, Hong A. Cancer-associated fibroblasts-derived exosomal miR-3656 promotes the development and progression of esophageal squamous cell carcinoma via the ACAP2/PI3K-AKT signaling pathway. Int J Biol Sci 2021; 17:3689-3701. [PMID: 34671193 PMCID: PMC8495391 DOI: 10.7150/ijbs.62571] [Citation(s) in RCA: 33] [Impact Index Per Article: 11.0] [Reference Citation Analysis] [Abstract] [Key Words] [MESH Headings] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 05/10/2021] [Accepted: 08/05/2021] [Indexed: 12/19/2022] Open
Abstract
Esophageal squamous cell carcinoma (ESCC) is one of the most common gastrointestinal tumors, accounting for almost half a million deaths per year. Cancer-associated fibroblasts (CAFs) are the major constituent of the tumor microenvironment (TME) and dramatically impact ESCC progression. Recent evidence suggests that exosomes derived from CAFs are able to transmit regulating signals and promote ESCC development. In this study, we compared different the component ratios of miRNAs in exosomes secreted by CAFs in tumors and with those from normal fibroblasts (NFs) in precancerous tissues. The mRNA level of hsa-miR-3656 was significantly upregulated in the former exosomes. Subsequently, by comparing tumor cell development in vitro and in vivo, we found that the proliferation, migration and invasion capabilities of ESCC cells were significantly improved when miR-3656 was present. Further target gene analysis confirmed ACAP2 was a target gene regulated by miR-3656 and exhibited a negative regulatory effect on tumor proliferation. Additionally, the downregulation of ACAP2 triggered by exosomal-derived miR-3656 further promotes the activation of the PI3K/AKT and β-catenin signaling pathways and ultimately improves the growth of ESCC cells both in vitro and in xenograft models. These results may represent a potential therapeutic target for ESCC and provide a new basis for clinical treatment plans.
Collapse
Affiliation(s)
- Yuan Jin
- Department of Cell Biology, College of Life Science and Technology, Jinan University, Guangzhou 510632, P. R. China
- National Engineering Research Center of Genetic Medicine, Guangzhou 510632, P. R. China
- Guangdong Province Key Laboratory of Bioengineering Medicine, Guangzhou 510632, P. R. China
- Guangdong Provincial biotechnology drug & Engineering Technology Research Center, Guangzhou 510632, P. R. China
| | - Qilin Meng
- Department of Cell Biology, College of Life Science and Technology, Jinan University, Guangzhou 510632, P. R. China
- National Engineering Research Center of Genetic Medicine, Guangzhou 510632, P. R. China
- Guangdong Province Key Laboratory of Bioengineering Medicine, Guangzhou 510632, P. R. China
- Guangdong Provincial biotechnology drug & Engineering Technology Research Center, Guangzhou 510632, P. R. China
| | - Bihui Zhang
- Department of Cell Biology, College of Life Science and Technology, Jinan University, Guangzhou 510632, P. R. China
- National Engineering Research Center of Genetic Medicine, Guangzhou 510632, P. R. China
- Guangdong Province Key Laboratory of Bioengineering Medicine, Guangzhou 510632, P. R. China
- Guangdong Provincial biotechnology drug & Engineering Technology Research Center, Guangzhou 510632, P. R. China
| | - Chen Xie
- Department of Cell Biology, College of Life Science and Technology, Jinan University, Guangzhou 510632, P. R. China
- National Engineering Research Center of Genetic Medicine, Guangzhou 510632, P. R. China
- Guangdong Province Key Laboratory of Bioengineering Medicine, Guangzhou 510632, P. R. China
- Guangdong Provincial biotechnology drug & Engineering Technology Research Center, Guangzhou 510632, P. R. China
| | - Xue Chen
- Department of Cell Biology, College of Life Science and Technology, Jinan University, Guangzhou 510632, P. R. China
- National Engineering Research Center of Genetic Medicine, Guangzhou 510632, P. R. China
- Guangdong Province Key Laboratory of Bioengineering Medicine, Guangzhou 510632, P. R. China
- Guangdong Provincial biotechnology drug & Engineering Technology Research Center, Guangzhou 510632, P. R. China
| | - Baoqing Tian
- Department of Cell Biology, College of Life Science and Technology, Jinan University, Guangzhou 510632, P. R. China
- National Engineering Research Center of Genetic Medicine, Guangzhou 510632, P. R. China
- Guangdong Province Key Laboratory of Bioengineering Medicine, Guangzhou 510632, P. R. China
- Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, Jinan, P. R. China
| | - Jiakang Wang
- Cancer Center of Guangzhou Medical University, Guangzhou 510090, P. R. China
| | - Tsung-Chieh Shih
- Department of Biochemistry and Molecular Medicine, University of California Davis, Sacramento, California, USA
| | - Yibo Zhang
- Department of Cell Biology, College of Life Science and Technology, Jinan University, Guangzhou 510632, P. R. China
- National Engineering Research Center of Genetic Medicine, Guangzhou 510632, P. R. China
- Guangdong Province Key Laboratory of Bioengineering Medicine, Guangzhou 510632, P. R. China
- Guangdong Provincial biotechnology drug & Engineering Technology Research Center, Guangzhou 510632, P. R. China
| | - Jieqiong Cao
- Department of Cell Biology, College of Life Science and Technology, Jinan University, Guangzhou 510632, P. R. China
- National Engineering Research Center of Genetic Medicine, Guangzhou 510632, P. R. China
- Guangdong Province Key Laboratory of Bioengineering Medicine, Guangzhou 510632, P. R. China
- Guangdong Provincial biotechnology drug & Engineering Technology Research Center, Guangzhou 510632, P. R. China
| | - Yiqi Yang
- Department of Cell Biology, College of Life Science and Technology, Jinan University, Guangzhou 510632, P. R. China
- National Engineering Research Center of Genetic Medicine, Guangzhou 510632, P. R. China
- Guangdong Province Key Laboratory of Bioengineering Medicine, Guangzhou 510632, P. R. China
- Guangdong Provincial biotechnology drug & Engineering Technology Research Center, Guangzhou 510632, P. R. China
| | - Size Chen
- Oncology Department, The First Affiliated Hospital of Guangdong Pharmaceutical University, Guangzhou 510080, P. R. China
- Guangdong Provincial Engineering Research Center for Precise Therapy of Esophageal Cancer, Guangzhou 510080, P. R. China
| | - Xinyuan Guan
- Department of Clinical Oncology, University of Hong Kong, Hong Kong, P. R. China
| | - Xiaojia Chen
- Department of Cell Biology, College of Life Science and Technology, Jinan University, Guangzhou 510632, P. R. China
- National Engineering Research Center of Genetic Medicine, Guangzhou 510632, P. R. China
- Guangdong Province Key Laboratory of Bioengineering Medicine, Guangzhou 510632, P. R. China
- Guangdong Provincial biotechnology drug & Engineering Technology Research Center, Guangzhou 510632, P. R. China
- ✉ Corresponding author: Dr. An Hong and Dr. Xiaojia Chen. (AH) , (XC)
| | - An Hong
- Department of Cell Biology, College of Life Science and Technology, Jinan University, Guangzhou 510632, P. R. China
- National Engineering Research Center of Genetic Medicine, Guangzhou 510632, P. R. China
- Guangdong Province Key Laboratory of Bioengineering Medicine, Guangzhou 510632, P. R. China
- Guangdong Provincial biotechnology drug & Engineering Technology Research Center, Guangzhou 510632, P. R. China
- ✉ Corresponding author: Dr. An Hong and Dr. Xiaojia Chen. (AH) , (XC)
| |
Collapse
|
|
48
|
Sunami Y, Häußler J, Kleeff J. Cellular Heterogeneity of Pancreatic Stellate Cells, Mesenchymal Stem Cells, and Cancer-Associated Fibroblasts in Pancreatic Cancer. Cancers (Basel) 2020; 12:cancers12123770. [PMID: 33333727 PMCID: PMC7765115 DOI: 10.3390/cancers12123770] [Citation(s) in RCA: 29] [Impact Index Per Article: 7.3] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Download PDF] [Figures] [Journal Information] [Subscribe] [Scholar Register] [Received: 11/10/2020] [Revised: 12/10/2020] [Accepted: 12/11/2020] [Indexed: 12/24/2022] Open
Abstract
Pancreatic cancer is projected to become the second deadliest cancer by 2030 in the United States, and the overall five-year survival rate stands still at around 9%. The stroma compartment can make up more than 90% of the pancreatic tumor mass, contributing to the hypoxic tumor microenvironment. The dense stroma with extracellular matrix proteins can be a physical and metabolic barrier reducing therapeutic efficacy. Cancer-associated fibroblasts are a source of extracellular matrix proteins. Therefore, targeting these cells, or extracellular matrix proteins, have been considered as therapeutic strategies. However, several studies show that deletion of cancer-associated fibroblasts may have tumor-promoting effects. Cancer-associated fibroblasts are derived from a variety of different cell types, such as pancreatic stellate cells and mesenchymal stem cells, and constitute a diverse cell population consisting of several functionally heterogeneous subtypes. Several subtypes of cancer-associated fibroblasts exhibit a tumor-restraining function. This review article summarizes recent findings regarding origin and functional heterogeneity of tumor-promoting as well as tumor-restraining cancer-associated fibroblasts. A better understanding of cancer-associated fibroblast heterogeneity could provide more specific and personalized therapies for pancreatic cancer patients in the future.
Collapse
|
|
49
|
Sueyama T, Kajiwara Y, Mochizuki S, Shimazaki H, Shinto E, Hase K, Ueno H. Periostin as a key molecule defining desmoplastic environment in colorectal cancer. Virchows Arch 2020; 478:865-874. [PMID: 33215229 DOI: 10.1007/s00428-020-02965-8] [Citation(s) in RCA: 12] [Impact Index Per Article: 3.0] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 03/18/2020] [Revised: 10/26/2020] [Accepted: 11/01/2020] [Indexed: 11/30/2022]
Abstract
Categorizing desmoplastic reaction (DR) based on the histological findings of cancer-associated fibroblasts is shown to be a promising novel method to predict prognosis of patients with colorectal cancer (CRC). Periostin (POSTN) in cancer-associated stroma is reportedly associated with poor clinical outcomes. Immunohistochemical staining with an anti-POSTN antibody was performed in 73 patients with pStage III CRC (cohort 1). In addition, to evaluate mRNA and protein expression levels of POSTN, we analyzed paired normal and invasive cancer frozen specimens by quantitative real-time polymerase chain reaction and western blot analysis in 41 patients (cohort 2). In cohort 1, according to the DR categorization, 18, 22, and 33 patients were classified as immature, intermediate, and mature, respectively. High immunoreactivity of POSTN was observed 100%, 68.2%, and 27.3%, respectively (p < 0.0001). The 5-year relapse-free survival rates were 56.8% and 82.7% in high and low POSTN expression subgroups, respectively (p = 0.015). In cohort 2, the POSTN mRNA and protein levels were significantly higher in the immature stroma as compared to the stroma characterized as other DR patterns. POSTN expression was closely associated with DR categorization. POSTN may be a key molecule that contributes to the malignant potential of CRC.
Collapse
Affiliation(s)
- Takahiro Sueyama
- Department of Surgery, National Defense Medical College, 3-2, Namiki, Tokorozawa, Saitama, 359-8513, Japan
| | - Yoshiki Kajiwara
- Department of Surgery, National Defense Medical College, 3-2, Namiki, Tokorozawa, Saitama, 359-8513, Japan.
| | - Satsuki Mochizuki
- Department of Surgery, National Defense Medical College, 3-2, Namiki, Tokorozawa, Saitama, 359-8513, Japan
| | - Hideyuki Shimazaki
- Department of Laboratory Medicine, National Defense Medical College, Tokorozawa, Japan
| | - Eiji Shinto
- Department of Surgery, National Defense Medical College, 3-2, Namiki, Tokorozawa, Saitama, 359-8513, Japan
| | - Kazuo Hase
- Department of Surgery, National Defense Medical College, 3-2, Namiki, Tokorozawa, Saitama, 359-8513, Japan
| | - Hideki Ueno
- Department of Surgery, National Defense Medical College, 3-2, Namiki, Tokorozawa, Saitama, 359-8513, Japan
| |
Collapse
|
|
50
|
Liao HY, Da CM, Wu ZL, Zhang HH. Ski: Double roles in cancers. Clin Biochem 2020; 87:1-12. [PMID: 33188772 DOI: 10.1016/j.clinbiochem.2020.10.015] [Citation(s) in RCA: 6] [Impact Index Per Article: 1.5] [Reference Citation Analysis] [Abstract] [Key Words] [Track Full Text] [Journal Information] [Subscribe] [Scholar Register] [Received: 08/13/2020] [Revised: 10/29/2020] [Accepted: 10/31/2020] [Indexed: 02/07/2023]
Abstract
The Ski (Sloan-Kettering Institute) is an evolutionarily conserved protein that plays a dual role as an oncoprotein and tumor suppressor gene in the development of human cancer. The Ski oncogene was first identified as a transforming protein of the avian Sloan-Kettering retrovirus in 1986. Since its discovery, Ski has been identified as a carcinogenic regulator in a variety of malignant tumors. Later, it was reported that Ski regulates the occurrence and development of some cancers by acting as an oncogene. Ski mediates the proliferation, differentiation, metastasis, and invasion of numerous cancer cells through various mechanisms. Several studies have shown that Ski expression is correlated with the clinical characteristics of cancer patients and is a promising biomarker and therapeutic target for cancer. In this review, we summarize the mechanisms and potential clinical implications of Ski in dimorphism, cancer occurrence, and progression in various types of cancer.
Collapse
Affiliation(s)
- Hai-Yang Liao
- The Second Clinical Medical College of Lanzhou University, 82 Cuiying Men, Lanzhou 730030, PR China; Orthopaedics Key Laboratory of Gansu Province, Lanzhou 730000, PR China
| | - Chao-Ming Da
- The Second Clinical Medical College of Lanzhou University, 82 Cuiying Men, Lanzhou 730030, PR China; Orthopaedics Key Laboratory of Gansu Province, Lanzhou 730000, PR China
| | - Zuo-Long Wu
- The Second Clinical Medical College of Lanzhou University, 82 Cuiying Men, Lanzhou 730030, PR China; Orthopaedics Key Laboratory of Gansu Province, Lanzhou 730000, PR China
| | - Hai-Hong Zhang
- The Second Clinical Medical College of Lanzhou University, 82 Cuiying Men, Lanzhou 730030, PR China; Orthopaedics Key Laboratory of Gansu Province, Lanzhou 730000, PR China.
| |
Collapse
|